Nebula Genomics DNA Report for Cavities
Are cavities, which result from tooth decay, genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

Table of contents
What are Cavities?
Dental cavities, also known as dental caries or tooth decay, are a prevalent oral health issue affecting people of all ages. While experts commonly associated them with poor oral hygiene and dietary habits, growing evidence suggests that genetic factors may contribute to an individual’s susceptibility to dental caries.
This article aims to explore the role of genetics in the development of cavities and shed light on the interplay between genetic predisposition and other factors that influence the health of your teeth.
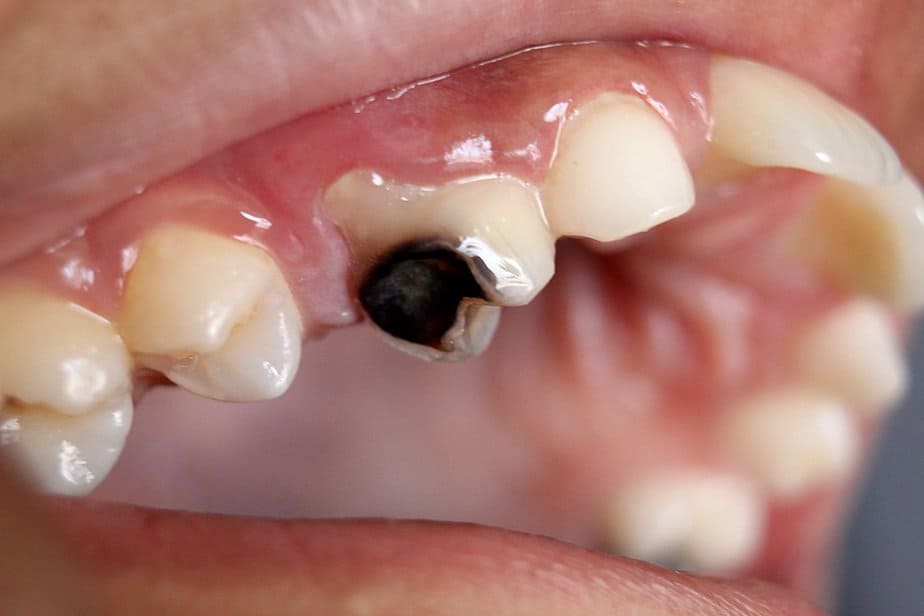
Cavities are areas of damage or holes in the teeth caused by tooth decay. They occur when acid-producing bacteria in your mouth demineralize enamel, the protective outer layer of the teeth, and form plaque. This demineralization weakens the enamel, leading to the formation of small holes or cavities. If left untreated, they can progress, affecting deeper layers of the tooth, including nerves and blood vessels, and potentially cause pain, infection, and tooth loss.
Tooth decay can alo lead to more serious problems such as gum disease or dental abscesses.
Types of cavities include smooth surface, pit and fissure, or root.
The best ways to prevent tooth decay involve brushing teeth twice a day with fluoride toothpaste or after eating and drinking, going to the dentist regularly, limiting snacking or sipping, and considering professional fluoride treatment to supplement this vital mineral.
Are Cavities Genetic?
While lifestyle factors and oral hygiene practices are primary determinants of cavity development, studies have shown that an individual’s susceptibility to cavities may be due to genetic factors. Some experts believe that up to 60 percent of tooth decay derives from genetics.
Scientists have identified several genetic factors that may play a role in making individuals prone to cavities.
- AMELX (Amelogenin X): The AMELX gene contributes to enamel formation during tooth development. Variations in this gene have been associated with enamel defects, such as amelogenesis imperfecta, which can increase the risk of compromised enamel structure.
- DSPP (Dentin Sialophosphoprotein): The DSPP gene is essential for dentin formation, which is the layer beneath the enamel. Variations in the genetics of this variant have been linked to dentin defects, such as dentinogenesis imperfecta, which can make teeth more susceptible to cavities.
- ENAM (Enamelin): The ENAM gene plays a crucial role in enamel development and mineralization. Mutations in this gene have been associated with enamel hypoplasia, a condition characterized by thin or insufficient enamel.
- AQP5 (Aquaporin-5) and CDHR2 (Cadherin-Related Family Member 2): These genes are involved in the formation of salivary glands and the production of saliva, which helps protect against cavities. Variations in this gene have been associated with reduced salivary flow, which can impact the oral environment and increase the risk of cavities.
- DEFB1: This gene is part of the body’s immune response system. Genetic variants are associated with a greater susceptibility to be infected by oral pathogens, increasing the risk of cavities by up to five times.
Epidemiology
Dental cavities are a global health concern, affecting a significant portion of the population. The prevalence of cavities varies across different age groups, regions, and socioeconomic backgrounds. According to the World Health Organization (WHO), dental cavities are among the most common chronic conditions worldwide, with an estimated 3.5 billion people affected by caries of permanent teeth.
Dental caries are even more prevalent in children, with nearly 60-90% of school-age children experiencing cavities. The burden of cavities remains a public health challenge, leading to various consequences on oral health and quality of life.
Symptoms
The symptoms of cavities can vary depending on the severity and location of the decay. In the early stages, cavities may not cause noticeable symptoms. However, as the decay progresses, cavities can lead to pain and infection that affect eating and speaking. Some common symptoms include:
Toothache: Pain or sensitivity in the affected tooth, which can be mild to severe, particularly while eating or drinking hot, cold, or sweet substances.

Tooth sensitivity: Increased sensitivity to hot or cold temperatures or sweet foods and beverages.
Visible holes or pits: Visible signs of decay, such as dark spots, pits, or holes on the tooth surface.
Tooth discoloration: Darkening or staining of the tooth surface.
Bad breath: Persistent bad breath or an unpleasant taste in the mouth.
Tooth sensitivity to pressure: Discomfort or pain when biting or applying pressure on the affected tooth.
Causes
The development of cavities is multifactorial, involving various factors that contribute to the decay process.
Experts commonly associate certain oral bacteria, particularly Streptococcus mutans, with cavity development. These bacteria produce acid as they feed on sugars and carbohydrates from the diet. The acid erodes the tooth enamel, leading to cavity formation.
A diet high in sugary drinks and acidic foods promotes bacterial growth and acid production in the mouth. Frequent consumption of such foods and inadequate oral hygiene lead to a higher risk.
Inadequate oral hygiene practices, such as infrequent or improper brushing and flossing, allow bacterial plaque to accumulate on the tooth surfaces. Plaque provides a favorable environment for bacterial growth and acid production, increasing the risk of cavities.
In addition to modifiable factors, such as oral hygiene and diet, some non-modifiable factors may also play a role. Saliva helps neutralize acids and remineralize the teeth, providing a natural defense against cavities. Reduced saliva flow or dry mouth conditions can impair the protective mechanisms, increasing the risk of tooth decay.
The structure and composition of teeth can also influence cavity susceptibility. Factors such as enamel thickness, enamel defects, and the shape and arrangement of teeth can affect the likelihood of cavity formation.
Diagnosis
Dentists can diagnose cavities and assess their severity. First, they will often ask about tooth pain and sensitivity before performing a dental examination. They will visually inspect the teeth for visible signs of decay, such as discoloration, holes, or pits on the tooth surfaces. Additionally, they may use dental explorers or probes to check for soft areas on the tooth surfaces, indicating decay.
To confirm a diagnosis or assess the extent of damage, dentists will often perform dental X-rays. These images help detect cavities that may not be visible to the naked eye, particularly in between the teeth or beneath existing fillings.
Treatment
Regular checkups can help catch cavities while they are still minor, preventing major symptoms or problems.
The treatment of cavities aims to remove the decayed tooth structure and restore the affected tooth. Appropriate treatment depends on the severity and extent of the cavity. Common treatment options include:
- Fillings: This is the main treatment option for cavities. After removing the decayed portion of the tooth, dentists fill the cavity with materials such as composite resin, amalgam, or porcelain to restore the tooth’s structure and function.
- Crowns: If there is extensive decay or weakening, a dentist may place a dental crown, a custom-fitted covering that replaces the tooth’s entire natural crown. These tools are made of gold, high strength porcelain, resin, porcelain fused to metal or other materials.
- Root canal: When decay reaches the tooth’s pulp, or inner material, a root canal may be necessary to save the remaining tooth. A dentist will remove the pulp, disinfect the root canal if infected, and replace the pulp with a filling.
Extraction: In severe cases where the tooth is extensively decayed or damaged, dentists may need to remove the tooth. The extracted tooth can be replaced with a dental implant or a prosthetic tooth.
Prevention
There are several ways to prevent cavities. The American Dental Association recommends maintaining good oral hygiene practices, avoiding sugary foods and drinks, and seeking regular dental health are key preventive measures. Additionally, dental professionals may recommend professional fluoride treatments that help strengthen tooth enamel and make it more resistant to acid attacks or dental sealants applied to the chewing surfaces of the back teeth to create a protective barrier.
If you liked this article, you should check out our other posts in the Nebula Research Library!
July 25, 2025
