The liver, a vital organ nestled beneath the ribcage, plays a crucial role in eliminating toxins from the body by filtering blood. The liver also produces bile, aiding in food digestion.
Early symptoms of liver disease, such as fatigue, abdominal pain and swelling, dark urine, and nausea or vomiting, can often go unnoticed or be misattributed. A distinctive symptom, however, is jaundice, characterized by a yellowish tint to the skin and eyes.
Liver disease can either be inherited or acquired due to factors such as viral infections, alcohol consumption, and obesity. The latter can lead to nonalcoholic fatty liver disease or nonalcoholic steatohepatitis, typically resulting from fat accumulation in the liver. This can then cause scarring (cirrhosis), a precursor to liver failure, which is a life-threatening condition.
Recent research has shed light on the role of genetics in liver disease. While several genetic variants linked to liver disease risk have been identified in the past, a recent study published in The New England Journal of Medicine suggests the existence of rare genetic variants that may offer protection against liver disease, including in obese individuals who are at increased risk.
| You can use the Nebula Genome Browser and Gene Analysis Tool to find this gene and see if you have these functional variants. Keep reading to learn what these mutations are and how you can check your status. |
The Study
The study involved exome sequencing in over half a million participants, with the aim of identifying associations between rare coding alleles and liver phenotypes. Overall, the analysis discovered mutations in the CIDEB gene as potential protective factors against liver disease.
The study involved 542,904 participants of diverse ethnic backgrounds, with a majority of European descent. At first, the researchers primarily sought to establish connections between genetic variants and biomarkers for liver damage. To accomplish this, they started at the gene level, narrowing down candidates to 13 associated genes.
Further analysis focusing on associations with liver disease reduced the list to five relevant genes. Finally, this process revealed four genes associated with a higher risk of nonalcoholic liver disease as well as variants in a single gene, CIDEB, that seemed to offer protection.
Further analysis of CIDEB mutations revealed that individuals carrying some combinations of truncating variants that affect various protein domains had a 31-54% lower likelihood of developing liver disease. These individuals also exhibited a reduced risk of cirrhosis and liver cancer.
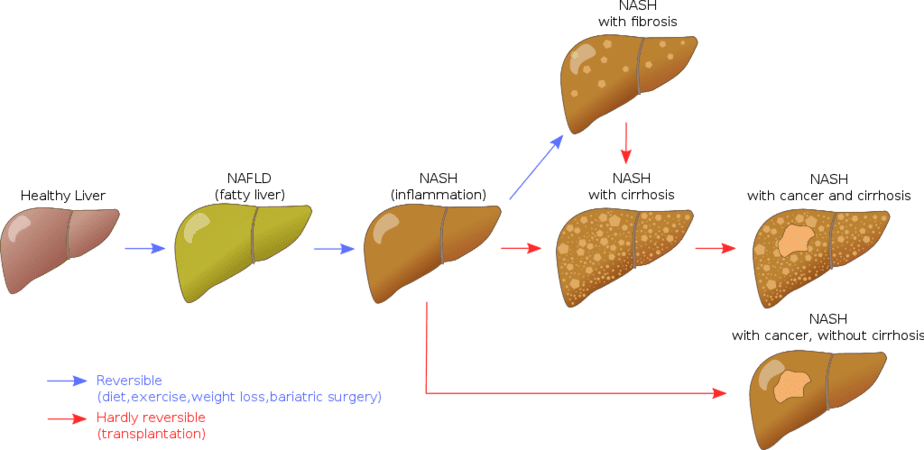
Given that obesity is a significant risk factor for non-alcoholic fatty liver disease, the researchers also investigated the effect of CIDEB mutations in obese individuals. They found that individuals with high BMI and CIDEB mutations exhibited a lower prevalence of liver disease.
Conclusions
In conclusion, the study found that rare CIDEB mutations were associated with lower biomarker levels indicative of liver damage and reduced odds liver disease. These findings could potentially play a role in future drug development, with the authors suggesting that inhibiting CIDEB could provide new therapeutic targets for treating nonalcoholic, fatty, and other types of liver diseases.
However, the study does have limitations. The genetic analysis was predominantly focused on individuals of European ancestry, leaving other ethnic groups underrepresented. Additionally, the authors recommend a larger study to better estimate the effect of CIDEB mutations on liver disease.
Overall, the study suggests that CIDEB mutations, although rare in the general population (less than 1%), are associated with a significantly lower chance of developing liver disease. It’s important to note that these protective variants are uncommon, meaning it’s typical for individuals not to carry them. These findings open new avenues for understanding the genetic factors influencing liver disease and also offer hope for future therapeutic interventions.
Explore your Genome!
Genome Browser
Did you know you can use the Nebula Genome Browser (available with Deep and Ultra Deep WGS) to check whether you have this protective variant?
- Go to the Genome Browser. In the top left corner of the genome browser, you can find a search bar.
- The authors identified multiple independent variants in CIDEB that contribute to protection. Four examples are rs138992080, rs371144775, rs765339323, and rs148553609.
- Using the dbSNP database, you can find the genome coordinates in the format [chromosome number][chromosome location] are 14:24305671, 14:24305686, 14:24305733, and 14:24306062. (GRCh38 reference genome).
- Copy-paste one of these locations into the search bar and press enter.
- The genome browser will now zoom in on these locations.
- Activate the “Center Line” in the bar at the top to better see the location that you are looking at.
- You should see stacked, gray stripes. Those are your personal DNA sequencing reads that are aligned to a reference genome sequence (colored letters above). If your DNA sequence matches the reference, then the stripes are gray. If the sequence is somehow different from the reference, then you will see various letters and symbols in different colors.
- The four variants, their locations and protective alleles are shown in the table below:
| rsID | Location (GRCh38) | Reference allele | Protective allele |
| rs138992080 | 14:24305671 | C | T |
| rs371144775 | 14:24305686 | C | G |
| rs765339323 | 14:24305733 | T | C |
| rs148553609 | 14:24306062 | C | T |
Gene Analysis Tool
You can also use the Nebula Gene Analysis Tool (available with Deep and Ultra Deep WGS) to see whether it flags any additional variants.
This tool empowers you to examine any gene in your genome and identify important genetic variants and mutations.
- When you click on the “Get Started” button your VCF file will be loaded into the Gene Analysis tool in a new tab.
- Type “CIDEB” into the search bar at the top.
- The Gene Analysis tool will extract genetic variants in the CIDEB gene from your VCF file and display them to you using symbols that have different colors. The colors denote the potential importance of variants. The Gene Analysis tool determines this by referencing the ClinVar database and other resources.
- Any red and orange variants could potentially be important. Click on them to check if any of them are truncating variants like the ones described in the study described above.
Citation
Verweij N, Haas ME, Nielsen JB, Sosina OA, Kim M, Akbari P, De T, Hindy G, Bovijn J, Persaud T, Miloscio L, Germino M, Panagis L, Watanabe K, Mbatchou J, Jones M, LeBlanc M, Balasubramanian S, Lammert C, Enhörning S, Melander O, Carey DJ, Still CD, Mirshahi T, Rader DJ, Parasoglou P, Walls JR, Overton JD, Reid JG, Economides A, Cantor MN, Zambrowicz B, Murphy AJ, Abecasis GR, Ferreira MAR, Smagris E, Gusarova V, Sleeman M, Yancopoulos GD, Marchini J, Kang HM, Karalis K, Shuldiner AR, Della Gatta G, Locke AE, Baras A, Lotta LA. Germline Mutations in CIDEB and Protection against Liver Disease. N Engl J Med. 2022 Jul 28;387(4):332-344. doi: 10.1056/NEJMoa2117872. PMID: 35939579.
