Table of contents
Nebula Genomics DNA Report for Cleft Lip
Is cleft lip genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

What is Cleft Lip?
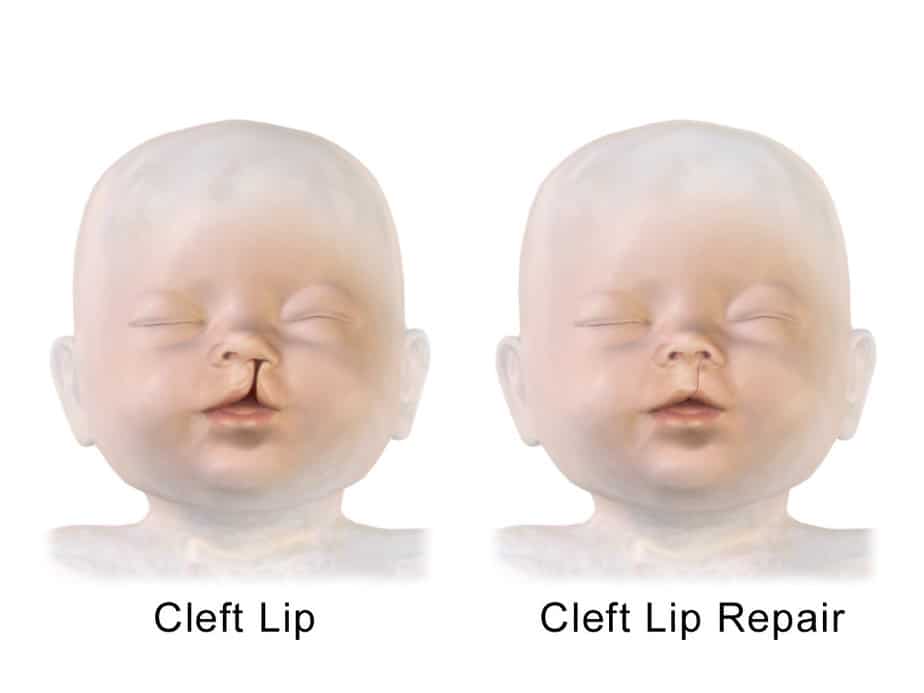
Cleft lip is part of a larger condition experts call orofacial cleft that includes both the lip and palate. The former occurs when there is a small notch or wider opening in the upper lip that may extend into the nose. It can happen on one or both sides of the nose or in the middle. Children with a cleft palate have an opening on the roof of the mouth (soft palate) that continues into the nose.
Children with these conditions often have feeding, speech, and hearing problems, plus frequent ear infections. They also lead to psychological and social problems if left untreated.
A cleft palate results from incomplete development of the tissues in the baby’s face making them not join completely. Experts are unsure of the cause in most cases, but certain risk factors involving the mother, including smoking and diabetes during pregnancy, appear to be associated with its development in the womb.
Doctors can diagnose the condition before birth. Early surgery within the first few months of life is often enough to correct the un-joined tissue. If treated, the child’s prognosis tends to be very good.
Is Cleft lip Genetic?
Experts have associated several genetic variants with cleft lip and palate syndromes. Since the condition tends to run in families, they suspect there is some heritable component. However, it is also possible that a mother’s environmental risk factors are common among family members.
Orofacial clefts often cause dental issues. Colgate notes some of the most common genetic factors associated with cleft lip that also affect tooth health, including Transforming growth factor-alpha (TGF-α), BCL3, DLX2, MSX1, TGFB3, and IRF6.
Overall, experts believe both genetic and environmental factors cause the condition. There are several other genetic variants identified specific to certain conditions involving cleft lip. Some of these candidate genes are:
- TP63
- RIPK4
- TFAP2A
- PVRL1
- CDH1
- PTCH1
- GLI2
- SHH
- SIX3
- TGIF
- FGFR1
- MID1
- GLI3
- OFD1
- IRF6
- WNT3
- PHF8
- MLL2, KDM6A
Researchers observe even more genes in patients with cleft palate alone. A genetic counselor may help a mother determine if the defect is caused by genetic factors.
Current Research on Cleft Lip Genetics
Parents and affected children have to deal with the psychological implications of cleft lip and palate. Therapies to this end include stimulating a positive attitude towards their child’s body and appearance. In 2018, two Saudi Arabian doctors evaluated the psychological effect of cleft lip and palate on children and their parents. They concluded that the condition causes distress to a child’s self-esteem and their parents’.
A more recent study by a large group of scientists attempted to study the mutations in IRF6, TFAP2A, and GRHL3, genes associated with cleft lip and palate. This is interesting to note since these genes are also present in mice and needed for their neurulation.
Although maternal smoking might increase the chances of the condition, further research is still needed. Last year, a systemic review and meta-analysis on maternal cigarette smoking and lip and cleft palate shed light on their relationship.
This interesting review paper from 2021 takes a deeper look at the prevalence of teeth agenesis among children with cleft lip or without cleft palate.
Epidemiology
Cleft lip and mouth palate are some of the most common birth defects in the world.
Overall, the condition is thought to affect 1 in 1000 births. However, that incidence is largely based on ethnicity, geography, and socioeconomic background. It is most common in Asia and the Americas and least common in Africa. Additionally, men tend to have a higher chance of developing cleft lip while women have a higher incidence of cleft palate.
A study in 2016 noted that the frequency of cleft palate varied significantly from 1.3 to 25.3 cases per 10,000 live births, with the highest rates in British Columbia, Canada, and the lowest rates in Nigeria, Africa.
Regardless of the incidence, girls had an increased risk compared to boys. This number agrees with the World Health Organization’s estimates, which also include the prevalence ranging 3.4 to 22.9 cases per 10,000 live births for cleft lip alone.
In the United States, 1 in 2,800 babies are born with cleft lip, 1 in 1,700 babies are born with cleft palate, and about 1 in 1,600 babies are born with both both conditions.
Symptoms
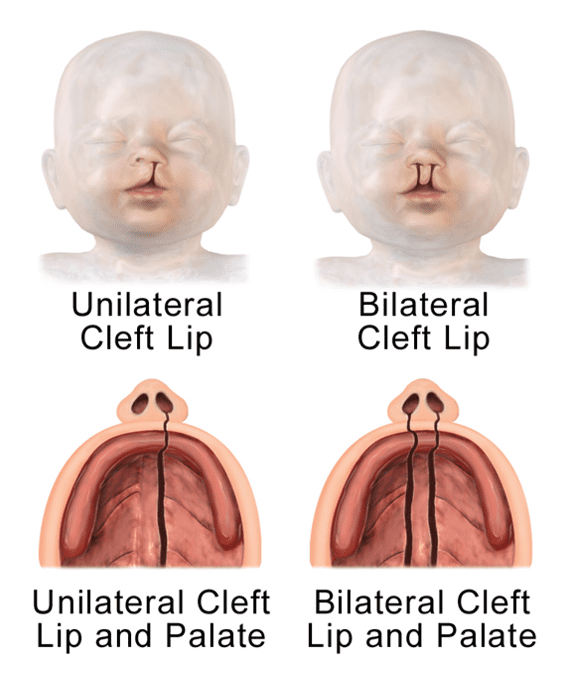
The most obvious symptom is a split in the upper lip or palate identified immediately after birth. Doctors can identify a cleft lip on an ultrasound, unlike cleft palate. Many babies are born with both conditions. The split can be unilateral (restricted to one side) or produce a bilateral cleft lip (encompassing both sides).
In addition to the physical signs, infants and children with cleft lip may also experience:
- Feeding issues (inability to latch or maintain consistent suck)
- Dental problems (crooked, poorly shaped or missing teeth)
- Speech problems and language difficulties
- Hearing impairment
- Social and self-esteem challenges
Causes
The definite cause of a baby with a cleft lip or palate is usually unknown. However, experts believe it is a combination of genetic and environmental exposures of the mother during pregnancy.
Around the fifth to sixth week of pregnancy, the two sides of the upper lip fuse together. At around 8 to 9 weeks, the roof of the mouth forms. The condition occurs when something interrupts the natural fusion, and a baby develops a split in this location.
Some environmental factors include:
- Maternal smoking or alcohol drinking during pregnancy
- The mother has diabetes
- Use of certain medications, such as those for epilepsy and anti-seizure drugs, during pregnancy
- Not enough folic acid during pregnancy
- Family history
Diagnosis
Doctors diagnose children born with cleft lip and cleft palate through visual observation shortly after birth. Sometimes, they can even diagnose the condition before birth through prenatal ultrasound.
An ultrasound will use soundwaves to take pictures of a fetus before birth. Through these images, doctors may be able to visualize facial structures. The condition will begin to be visible around the 13th week of pregnancy and become more evident as the pregnancy progresses. Cleft palate alone is more difficult, but not impossible, to diagnose before birth since it occurs inside the mouth and is harder to see on an ultrasound.
If cleft lip is observed, a mother may allow a sample of amniotic fluid to be taken from the uterus to test for genetics that may have caused the condition. However, in most cases of cleft lip and palate, the direct cause will remain unknown.
Treatment
Treating children with cleft lips or palates is designed to improve a child’s ability to eat, speak and hear normally and to achieve a normal facial appearance. Ultimately, surgery to repair the defect is the only cure. A team of medical professionals will usually include plastic surgeons, pediatricians, pediatric dentists, auditory or hearing specialists, speech therapists, and psychologists.
Surgery
Options will be provided based on the specific condition of the infant. In most cases, the first surgery will involve closing the split. Additional treatment to help speech and to further improve facial features may be necessary. Typical surgeries include:
- Cleft lip repair — within the first 3 to 6 months of age
- Cleft palate repair — by 12 months, or earlier if possible
- Follow-up surgeries — between age two and late teen years
For these surgeries, a child with cleft lip is placed under general anesthetic. Some procedures are:
- Strategies to repair a cleft lip: A surgeon makes incisions on both sides of the lip to create a flap that are stitched together to give the lip a more normal appearance and function. They also perform an initial nasal repair if needed.
- Strategies to repair a cleft palate: The surgeon will make incisions on both sides of the aperture and reposition the tissue and muscles to close the gap. They may use various procedures based on the specific condition.
- Ear tube surgery (cleft palate): Tiny ear tubes are placed in the eardrums to reduce the risk of hearing loss from chronic ear fluid.
Additional surgeries may be needed to improve the appearance of the mouth, lip, and nose. Risk factors associated with these surgeries include bleeding, infection, poor healing, widening or elevation of scars, and temporary or permanent damage to nerves, blood vessels or other structures.
The long term complications that accompany conditions like cleft lip and cleft palate may be treated through non-surgical means. Depending on the child’s case, your doctor may recommend:
- Feeding strategies
- Speech therapy
- Orthodontic treatment (such as braces)
- Monitoring and treatment for ear infections and hearing loss
- Hearing aids
- Psychology sessions
Other sources
You can visit the National Institutes of Health, the National Institute of Dental and Craniofacial Research website, or the Cleft Lip and Palate Association, where you can get involved in the research council.
If you liked this article, you should check out our other posts in the Nebula Research Library!
May 22, 2023
