Table of contents
Nebula Genomics DNA Report for CLL
Is CLL genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

| This information has been updated to reflect recent scientific research as of August 2021. |
This article covers information regarding chronic lymphocytic leukemia (CLL), a chronic form of leukemia that mainly affects adults over the age of 70. Check out our other articles for more information on other blood cancers (including Hodgkin lymphoma and non-Hodgkin lymphoma) and the other form of lymphocytic leukemia, acute lymphocytic leukemia (ALL), most common in children.
What is CLL?
All leukemias are diseases of the blood and bone marrow. CLL is a type of leukemia in which the bone marrow produces too many abnormal white blood cells called leukocytes. Specifically, CLL affects B leukocytes, which play an integral role in making antibodies that help the immune system fight infections. In some people with CLL, the immune system produces abnormal antibodies that attack normal cells, like red blood cells and platelets. This causes low blood cell counts.
Bone marrow produces all types of blood cells, including red blood cells, white blood cells, and platelets. The abnormal white blood cells produced during CLL do not function properly. Instead, they crowd out healthy cells in the bone marrow, replace normal leukocytes in the body, and accumulate in the blood and organs.
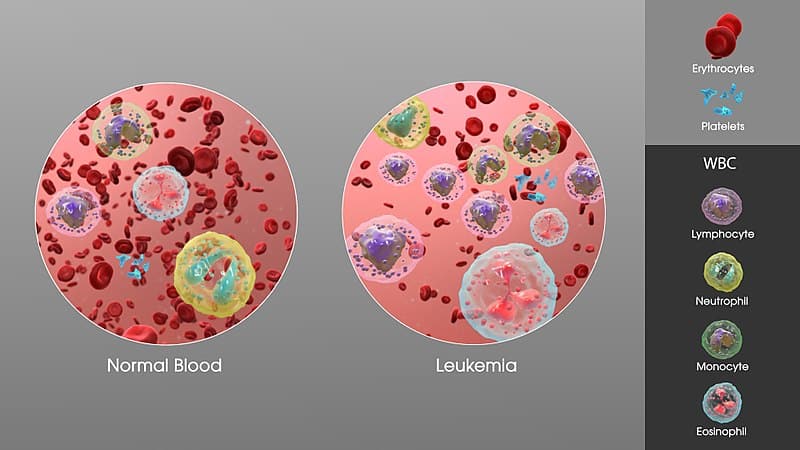
When the condition starts, it is not uncommon for patients to show little or no symptoms. However, as the disease progresses, symptoms become more pronounced. Because of this asymptomatic nature, many people are not diagnosed until years after the cancer starts. Once symptoms appear, they are usually noticed as enlarged lymph nodes, fatigue, fever, and weight loss. Enlargement of the spleen and anemia may also occur.
Diagnosis is often made using a blood test, and cancer treatment consists of a combination of radiation and chemotherapy. Relatively, the prognosis of this cancer is good, with a five-year survival rate of 83% after diagnosis.
Is CLL Genetic?
Sometimes, patients can inherit genetic mutations that increase the risk of CLL, but only in a small number of cases. The mutations that change the way bone marrow makes blood cells are genetic, but they are not hereditary. Thus, CLL is generally not thought of as a familial cancer.
This also means that risk factors like smoking or exposure to certain chemicals increase the likelihood of acquiring one of these mutations while family history of CLL has a very small impact. In other words, having a parent or sibling with the condition is not likely to increase your risk.
In CLL, the mutations are normally observed as chromosomal abnormalities, with approximately 80% of patients carrying at least 1 of the following alterations: missing segments, or deletions, in chromosomes 13, 11, or 17 or an extra copy of chromosome 12 (trisomy 12). Deletion in chromosome 13 tends to be associated with a better prognosis, while deletions in chromosomes 11 and 17 tend to be associated with a worse prognosis. Trisomy 12 seems to have no effect on the outlook.
According to this research study, published in 2017, certain gene mutations may indicate whether an individual will benefit from chemotherapy or not. Specifically, they found that a TP53 mutation or deletion results in poorer outcomes with chemotherapy, while IGHV mutations identify patients that benefit most from chemotherapy. This discovery has implications in how doctors prescribe treatment for this disease. Namely, starting patients with the TP53 alteration on treatments other than the standard chemotherapy.
Current Research on CLL
There have been several studies on whether CLL has a genetic predisposition.
According to a study carried out in 2009, the research authors claimed to have discovered an inherited susceptibility to chronic lymphocytic leukaemia. They found that approximately 10% of individuals with reports of CLL have a family member that has also experienced the condition or a related lymphoproliferative disorder (such as mantle cell lymphoma) that is a risk factor for CLL.
More detailed cancer research focused on familial clustering of chronic lymphocytic leukemia established that in certain cases, CLL follows a model similar to that of hereditary. However, the research, one of the few in-depth studies on CLL connection, was unable to confirm this hereditary model.
The author of the studies stated that from the observation of 100 families across seven decades, CLL clustering had been documented. While the clustering is not enough to say that CLL is hereditary, familial aggregation presented strong evidence that supports the role of many inherited genetic factors in the development of the disease.
A 2014 study titled “Genetic Abnormalities in Chronic Lymphocytic Leukemia: Where We Are and Where We Go” also tried to identify the connection between CLL and genetics. Researchers cited that next-generation sequencing (NGS) methods performed in the last few years have identified a wide range of gene mutations such as TP53, NOTCH1, SF3B1, and BIRC3 that have improved medical genetic professionals’ understanding of CLL development and the possibility of genes playing a role.
Most recent information cited by the American Cancer Society and others indicates that CLL is caused by acquired genetic mutations. Sometimes, parents can pass down certain mutations that increase the risk of certain types of cancer, but this is a rare occurrence. Changes in DNA caused by CLL normally occur during a person’s lifetime rather than inherited.
Epidemiology
CLL is most common in older adults with an average age of onset of around 70 years. About 9 out of 10 cases occur in patients over 50. It is extremely rare in children. It is slightly more common in males than in females. Ethnicity-wise, the disease affects more people in North America and Europe than in Asia.
In 2021, the American Cancer Society reported about 21,250 new cases of CLL and nearly 4,320 deaths contributed to the disease. Overall, it accounts for one-quarter of all new cases of leukemia. The average lifetime chance of developing the condition is 0.57% in someone with no risk factors. The risk of developing CLL increases if you are chronically exposed to things like smoking or certain chemicals.
Symptoms
When the cancer starts, it is common to have no signs or symptoms of the disease. In many cases, the condition is discovered when a patient receives a blood test for another issue, and high levels of leukocytes are found.
Symptoms may appear as the disease progresses but, they tend to be general:
- Weakness
- Feeling tired
- Weight loss
- Chills
- Fever
- Night sweats
- Swollen lymph nodes
- Bloating, which is caused by an enlarged spleen and/or liver
Since the abnormal white blood cells produced with CLL crowd out normal cells, patients experience certain conditions associated with low blood cell levels. These include anemia (low red blood cells), leukopenia (low normal white blood cells), and thrombocytopenia (low platelets).

Anemia causes tiredness, weakness, and shortness of breath, while leukopenia is most often associated with an increased risk of infections. Thrombocytopenia is characterized by excess bruising, bleeding, frequent or severe nosebleeds, and bleeding gums.
Generally, people with CLL will experience more frequent infections, especially those of the upper and lower respiratory tract. A number of people are also at an increased risk of developing cancer of other types, including large B-cell lymphoma and certain skin cancers.
Causes
The cause of CLL is unknown. However, it is known to be associated with a genetic mutation in the bone marrow that leads to ineffective white blood cells. Genetic tests can help assess a patient’s status.
The greatest risk factors of CLL are age (most cases are diagnosed in patients over 70) and gender, with males being slightly more at risk than females. Environmental factors are a risk as well. In particular, certain herbicides and insecticides, including Agent Orange used during the Vietnam War, have been linked to an increased risk of chronic lymphocytic leukemia.
Persons diagnosed with the non-cancerous condition, monoclonal b cell lymphocytosis may be at higher risk for CLL.
Diagnosis
Blood tests are the most common approach to diagnose CLL. Your health care provider will most likely perform a complete blood cell count. A differential is often also performed to measure the different kinds of white blood cells present.
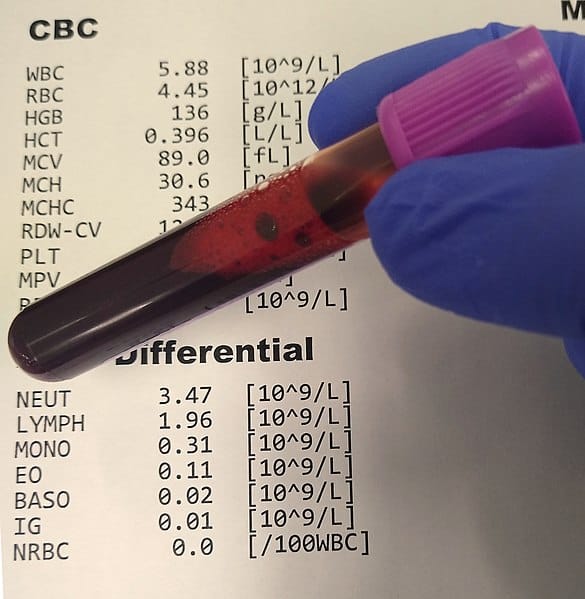
Patients with chronic lymphocytic leukemia will have too many lymphocytes. A value of more than 10,000 lymphocytes/mm³ (per cubic millimeter) of blood is usually a sign of CLL. Since these white blood cells prevent the presence of other blood cells, patients may also have low levels of red blood cells and platelets.
If CLL is suspected, flow cytometry will be performed in combination with the blood count. This instrument-based procedure will confirm if the extra lymphocytes are CLL cells and rule out other conditions, such as other blood disorders and infections.
Additional tests and procedures can help confirm diagnoses such as bone marrow aspiration and biopsy. Aspiration is the process of using a syringe and needle to remove about a small amount of liquid bone marrow for analysis. This procedure can be painful, even with numbing agents.
Biopsy is the process of removing bone and marrow, which may be uncomfortable, but usually doesn’t hurt. Then, the samples are viewed under a microscope and analyzed for size, shape, and other characteristics that identify the types of white blood cells present. This test can differentiate between CLL and the acute form of leukemia.
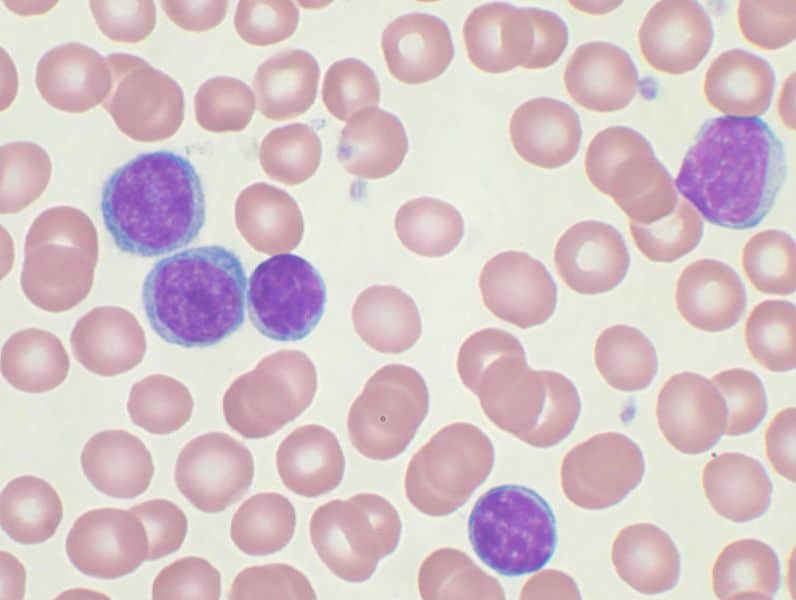
Some additional tests may be ordered not to diagnose CLL but to determine if the cancer is spreading. These include a lumbar puncture and imaging tests such as CT scans and PET imaging.
Treatment
CLL treatment is based on a number of factors that include cancer stage, your overall health, and personal preferences.
Early stage
Patients with an early stage of the disease are generally not treated as it has been shown that treatment in this stage does not improve overall outlook or extend life. Instead of putting patients through unnecessary treatments, your doctor will monitor the condition through regular blood tests until treatment is necessary through a process called watchful waiting. Patients can participate in clinical trials at this stage, mainly to determine if new early intervention strategies may be useful.
Intermediate and advanced stages
At these stages, your doctor will normally start traditional treatment options to improve your quality of life. They can be used alone or in combination. Mayo Clinic summarizes these treatments:
Chemotherapy: a drug treatment that kills quickly growing cells, including cancer cells. This medicine is available in injectable or oral forms. Chemotherapy drugs can be used alone or in combination to treat CLL.
Targeted drug therapy: The outside of cancer cells can be targeted using drugs designed specifically for identifying and killing them. The choice of therapy will depend on your specific cancer cells.
Immunotherapy: a treatment that uses your body’s immune system to fight cancer. Immunotherapy treatments train your natural immune system to recognize and destroy cancer cells.
Bone marrow transplant: A bone marrow transplant, or stem cell transplant, uses strong chemotherapy drugs to kill the stem cells in your bone marrow that are creating diseased lymphocytes. Then, healthy adult blood stem cells from a donor are infused so that they enter the bone marrow and begin making healthy blood cells.
Due to its complexity and the range of other effective options available, bone marrow transplants have become less common in recent years. They may still be an option for certain cases.
Throughout treatment, your doctor will usually monitor you for other conditions related to CLL, including certain types of cancers, vaccinations to reduce risk of infections, and other side effects and health problems. Support from family members can also help disease outlook.
Fatigue is one of the most common features of the condition. To help you cope with fatigue, you may be interested in alternative medicine techniques such as exercise, massage, meditation, relaxation, and yoga. You can often find specialists to assist with these therapies.
For more information, you should check out the National Cancer Institute, including the chronic lymphocytic leukemia treatment (PDQ) page, the Leukemia & Lymphoma Society, and the American Cancer Society websites.
If you liked this article, you should check out our other posts in the Nebula Research Library!
July 12, 2022
