Table of contents
Nebula Genomics DNA Report for Gout
Is gout genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

What is Gout?
Gout is a common and painful form of inflammatory arthritis in the joints. Most patients notice certain joints that are red, tender, hot, and swollen. The condition occurs quickly in what is known as flares that occur for one to two weeks.
Acute gout attacks usually resolve themselves on their own or with mild treatment. However, repeated occurrences can lead to a more serious condition called gouty arthritis.
It usually occurs in only one joint at a time and at least half of the cases occur in the joint at the base of the big toe. It may also result in tophi, kidney stones, or kidney damage.
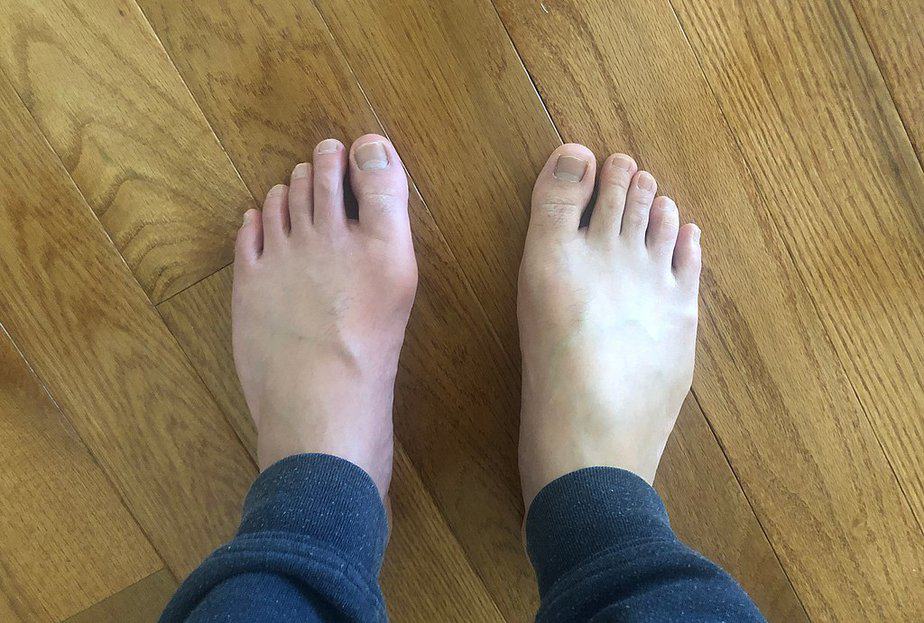
Sharp crystallization of excess uric acid in the joints, tendons, and surrounding tissues causes the condition. People who have a genetic predisposition or eat certain diets are at a higher risk of gout. Doctors diagnosis by confirming the presence of crystals in and around the joints or by measuring uric acid levels in the blood, which will be elevated around the time of a gout attack.
To treat gout, your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), glucocorticoids, or colchicine to reduce the symptoms. After an attack subsides, patients can implement lifestyle changes, mainly in the diet, to prevent a recurrence.
Is Gout Genetic?
Gout is most likely a result of complex genetic and environmental factors. Having a close family member with the condition increases an individual’s genetic risk.
Experts have shown that many genetic factors with small effects contribute to gout. The genes involved are those that transport, release, or reabsorb urate, transport or break down sugars, and transport other small molecules. The two genes that seem to have the greatest effect are:
SLC2A9: Encodes for a protein in the kidneys that manages the body’s levels of urate. It promotes both releasing urate into the urine or reabsorbing it into the bloodstream. When this genetic variation is affected, the body may release too little urate or reabsorb too much.
ABCG2: Encodes for a protein that helps release urate into the gut for removal from the body.
In 2017, a genetic study involving the meta analysis of gout in people with European ancestry identified nine loci associated with gout: ABCG2, SLC2A9, GCKR, MLXIPL, SLC17A1-A4, SLC16A9, SLC22A12, PDZK1, TRIM46. This study aligned with previous genome wide association studies that identified these areas as associated with high serum urate levels. These new and previous studies suggest a strong connection between the two conditions.
Additionally, in 2018, researchers at the University of Otago helped characterize a new linked variant, PDZK1.
Epidemiology
Gout is the most common type of arthritis in the general population and cases appear to be rising around the world. In the United States, experts believe prevalence has doubled between the 1960s and 1990s.
Depending on the population studied, prevalence ranges from <1% to 6.8%. In 2015-2016, prevalence in the United States was estimated to be 3.9% or 8.3 million people.
It is more common in men than in women and risk increases with age. More people will get it during middle age and it normally does not occur in women before menopause.
Symptoms
The most common gout symptom is intense joint pain and swelling, usually the big toe. Other symptoms of gout include:
- Redness
- Stiffness
- Swelling
- Tenderness
- Warmth, or a feeling like the joint is “on fire”
Experts refer to the appearance of symptoms as a flare. Gout flares usually last for one to two weeks before going into remission, or a time when no symptoms are present.
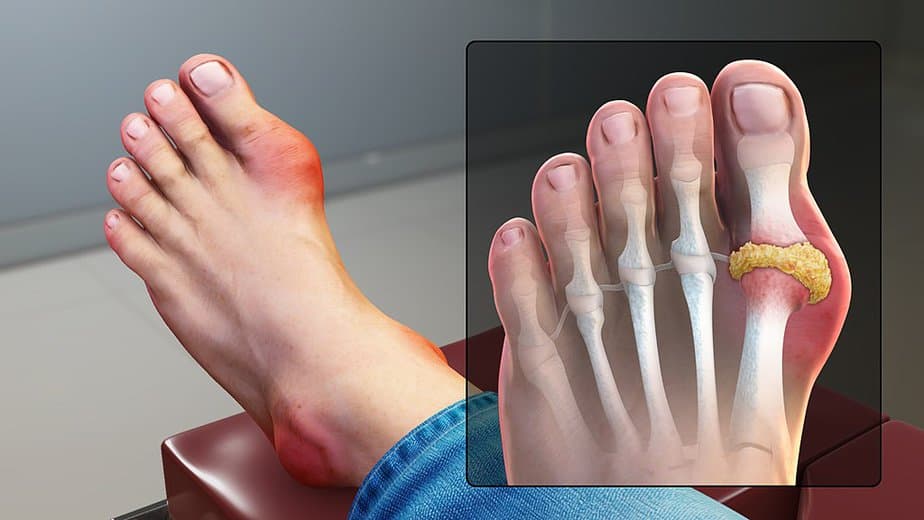
They can be frequent or infrequent, only occurring every few years. If left untreated, there is a greater chance the flares will be more frequent, severe, or spread to other areas of the body.
Some people with this condition develop other ailments of the heart and kidneys. For example, the urate crystals can accumulate in the kidneys and form kidney stones.
Causes
The biological cause of gout is having too much urate (uric acid) in the blood, also known as hyperuricemia. About one quarter of those with hyperuricemia will develop gout.
Urate is produced as a product of purine metabolism, a chemical in food and drink. It is a byproduct that the body normally removes in the kidneys.
If there is too much in the body or the kidneys are not effective at removing it, uric acid builds up forms needle-shaped crystals in the joints. This can result in activation of an inflammatory response at the site. Not everyone with high levels of uric acid crystals develops gout.
As noted by the National Institute of Arthritis and Musculoskeletal and Skin Diseases, risk factors that contribute to the condition are:
- A family history of gout
- Being older
- Drinking alcohol
- Eating foods purine rich foods (usually from animal sources), a substance that breaks down into urate
- Drinking beverages that have high-fructose corn syrup, such as soda
- Some health conditions, such as overweight or obesity, high blood pressure, and chronic kidney disease
- Some medications
Because the condition is associated with a rich diet, it used to be known as the “disease of kings” or “the rich man’s disease”.
Diagnosis
Diagnosing the condition is usually a straightforward process during which a doctor will examine the affected joint and interpret your symptoms. Additional tests may help confirm diagnosis, most of them focused on identifying urate in the joints:
Joint fluid test: A needle is used to draw fluid from an affected joint. The fluid is observed under a microscope to look for urate crystals.
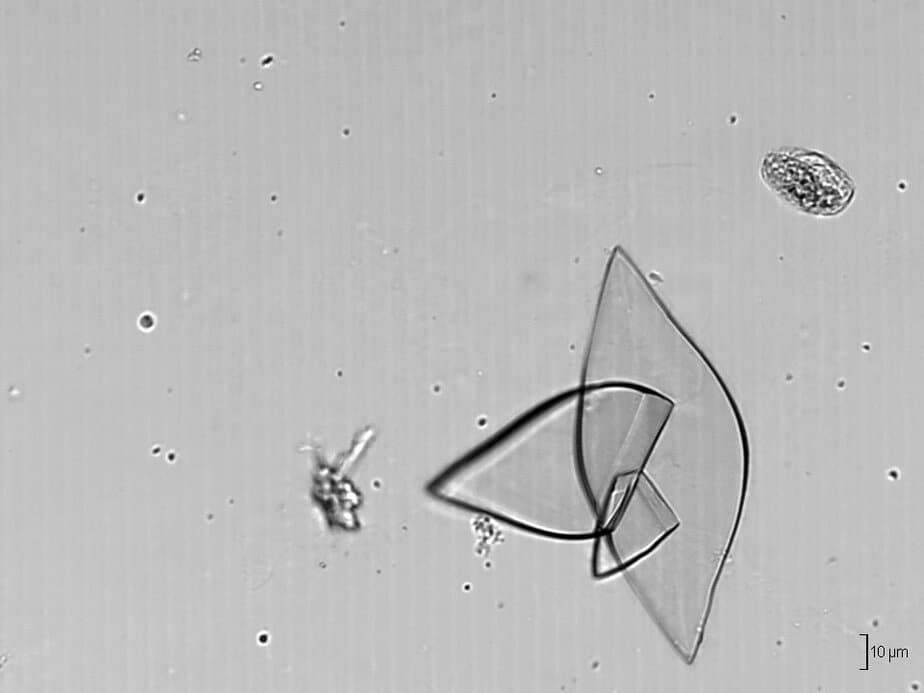
Blood test: Blood tests can be used to measure serum urate levels. An issue with these tests is that they may not accurately reflect the condition. While some people with gout have a buildup of uric acid, others may not. And some people with high levels do not have gout.
X-rays: These can be used to rule out other causes of joint inflammation.
Ultrasound: This imaging technique may detect urate crystals in joints or in tophi.
Dual-energy computerized tomography (DECT): This test combines X-ray images taken from many different angles to visualize urate crystals in joints.
Treatment
Treatment of gout may include two different types of medications as well as lifestyle changes.
Medications to treat symptoms
Nonsteroidal anti-inflammatory drugs (NSAIDs): NSAIDs include over-the-counter options such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve). Prescriptions may include indomethacin (Indocin, Tivorbex) or celecoxib (Celebrex). NSAIDs carry risks of stomach pain, bleeding and ulcers.
Colchicine: These are anti-inflammatory drugs that reduce gout pain. Side effects include nausea, vomiting and diarrhea.
Corticosteroids: Medications such as prednisone may control gout inflammation and pain. Side effects may include mood changes, increased blood sugar levels and elevated blood pressure.
Medications to lower uric acid
attacks. They can reduce complications and damage that has already occured due to the condition.
Medications that block uric acid production: These medications help limit the amount of uric acid your body makes. There are several side effects including fever, rash, nausea, hepatitis and kidney problems. Some medications may also affect the heart.
Medications that improve uric acid removal: These medications improve your kidneys’ ability to remove uric acid from your body. Side effects include a rash, stomach pain and kidney stones.
Lifestyle changes
While medications are important, changes in lifestyle provide means to reduce flares and improve the overall condition. Diet and exercise is usually key to success.
Beverages: Drink lots of water to help kidney function and avoid dehydration. Also, limit alcoholic beverages and drinks sweetened with fruit sugar (fructose).
Foods: Avoid foods high in purines, which can lead to uric acid buildup. This includes red meat and organ meat as well as seafood such as anchovies, sardines, mussels, scallops, trout, and tuna. Include low fat dairy as a substitute for these proteins.
Exercise: Exercise regularly and lose weight, if needed. A lower weight reduces pressure on joints, particularly weight bearing joints like the hips and knees. This can help manage many forms of arthritis. Low-impact activities such as walking, bicycling, and swimming can help reduce strain on the joints.
Medications: Change medications associated with hyperuricemia. These include diuretics or “water pills”. Some immunosuppressants may also increase risk for the condition.
More information can be found on the American College of Rheumatology website.
If you liked this article, you should check out our other posts in the Nebula Research Library!
June 2, 2023