Nebula Genomics DNA Report for Strokes
Are strokes genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

Table of contents
What are Strokes?
A stroke occurs when blood flow is reduced to parts of the brain and brain cells begin to die. Without proper blood flow, the brain cannot function correctly. There are various classifications of this condition based on where and how the reduced blood flow occurs. The two main types are ischemic (due to lack of blood flow, usually caused by a blocked blood vessel) and hemorrhagic (due to bleeding).
The most common symptoms include an inability to move or feel on one side of the body, problems understanding or speaking, dizziness, or loss of vision to one side. Hemorrhagic strokes are also associated with severe headaches. Sometimes, these symptoms last for only one or two hours, in which case the episode is referred to as a mini-stroke. Symptoms can become permanent and cause long term complications.
The main risk factor is high blood pressure. You may also be at higher risk if you have high cholesterol, smoking, obesity, diabetes mellitus, previous strokes, end-stage kidney disease, and atrial fibrillation.
Diagnosis is usually made through a physical exam and imaging such as a CT scan or MRI. Prevention includes reducing risk factors as well as surgeries and/or medication if you are determined to be at a higher risk.
A stroke is usually a medical emergency that requires immediate treatment. Medications and surgery can be performed if the condition is caught early enough, within the first few hours. After an episode, a patient may also require stroke rehabilitation to help regain loss of function.
Are Strokes Genetic?
If you have a close family member who has had a stroke, your risk is also elevated. In part, this can be attributed to some genetic factors. Additionally, members of the same family tend to share the same environment and may have similar habits that affect risk, such as smoking and an unhealthy diet. Cigarette smoke in particular reduces the amount of oxygen the blood is able to carry.
Because so much of the risk is associated with lifestyle factors, it has been difficult to identify specific genetic variants that may be contributing. Although some common individual genetic factors have been identified, their contribution to overall risk is modest. Most are linked to ischemic stroke:
TSPAN2: Affects vascular development and atherosclerosis
FOXF2: Causes small vessel diseases. This is the only variant related to both ischemic and hemorrhagic types
ABO: Linked to thrombosis
HDAC9: Linked to atherosclerosis
PITX2 and ZFHX3: Both related to atrial fibrillation
NOTCH3: CADASIL (Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy) is an autosomal dominantly inherited angiopathy caused by pathogenic variants in the NOTCH3 gene on chromosome 19. CADASIL is now recognized as an important cause of stroke in the young.
Genetic factors that cause conditions such as diabetes and high blood pressure are indirectly related to stroke since it is known that these conditions put patients at greater risk.
In most cases, the genetic risk of stroke is identified as genetic disorders in which a stroke is one of several manifestations, including sickle cell disease. Rare single gene disorders may contribute to individual familial syndromes for which stroke is the primary outcome. These include cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy.
Epidemiology
According to the Centers for Disease Control and Prevention (CDC), 1 in every 6 deaths from cardiovascular disease was due to stroke in 2018. Every year, more than 795,000 people in the United States have a stroke which is equivalent to 1 stroke every 40 seconds. About 87% are classified as ischemic strokes, resulting from blocked blood flow to the brain.
stroke is more common in certain ethnicities. Risk of having a first stroke is nearly twice as high for African Americans as for whites. Black persons also have the highest rate of death due to stroke. Deaths from the condition have fallen in recent years for most ethnicities, but have increased for Hispanic Americans.
Receiving emergency care as soon as possible after recognizing the condition is the best way to reduce disability and death.
While anyone can experience a stroke, they are more likely with increased age.
Symptoms
It’s important to recognize signs and symptoms of a stroke quickly, as prognosis is based on how quickly you can get emergency care. Quick action, within 3 hours of the start of symptoms, is the most important factor to reduce brain damage and can even save your life. There may be less options for treatment if you wait.
Symptoms of the condition are most likely recognized as what the American Stroke Association has labeled as the F.A.S.T. warning signs:
- Face-dropping
- Arm weakness
- Speech difficulty
- Time to call 911

People who have a stroke may have other signs include numbness or weakness in the face, arms, or legs, especially on one side of the body, confusion, vision problems, dizziness, and severe headache. The headache is more common during the hemorrhagic type.
You should note the time in which symptoms first appear to help emergency personnel determine the best treatment.
Symptoms that go away quickly are often referred to as a transient ischemic attack (TIA). Although not an emergency, this occurrence can be the sign of a serious medical condition that requires diagnosis and treatment. Anyone who thinks they may have had a TIA should contact their medical provider as soon as possible.
Causes
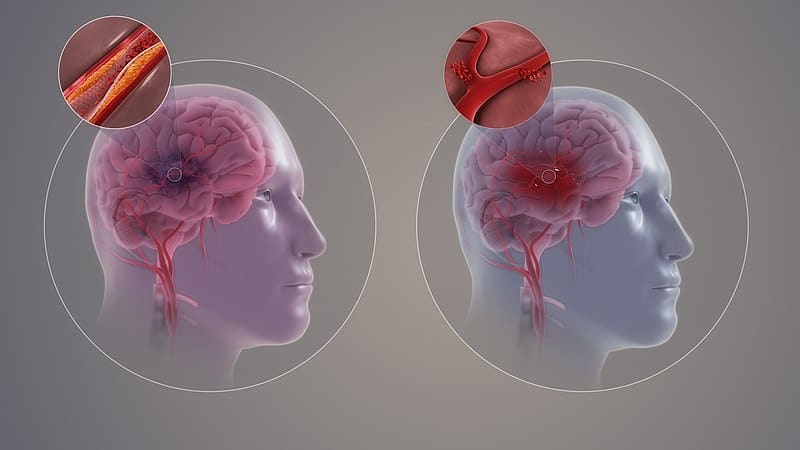
The two main types of stroke, ischemic and hemorrhagic are caused by different mechanisms.
Ischemic
This is the most common type of stroke. It is caused when blood supply is blocked from the brain, usually by blood clots. These clots can form when atherosclerosis, a condition that causes fatty deposits called plaque to narrow or block arteries, occurs in other parts of the body. That plaque can break off, leading to the blood clot that ultimately blocks blood to the brain.
While age can contribute to the narrowing of blood vessels over time, risk factors for stroke such as high blood pressure and diabetes, increase the chances of it occurring. Controlling these factors are an important component to prevent a stroke.
Heart disease and irregular heart beat, also known as atrial fibrillation, can also cause this type of stroke. In this case, the blood clot forms in the heart before breaking off and affecting the blood vessels to the brain.
Hemorrhagic
These are less common than the ischemic type. They can occur when a blood vessel inside the skull bursts and bleeds into and around the brain. High blood pressure is the greatest risk factor as it can weaken the blood vessels in and around the brain, causing them to break more easily.
In addition to the most common risk factors, lack of exercise and stress can also affect the occurrence. Brain aneurysms and abnormally formed blood vessels in the brain are also risk factors.
A person is more likely to experience either type of stroke if you are older than 55. However, about 25% of the occurrences occur in younger people. Family history of stroke and ethnicity also increase your risk. Finally, those who have other conditions, such as a TIA or heart attack are also at higher risk for having a stroke.
Diagnosis
Because stroke is a medical emergency, diagnostic tests are performed immediately once you arrive at the hospital. Although doctors can usually recognize a stroke by the signs and symptoms, they will perform a series of tests immediately to determine what kind of stroke it is, which will affect treatment.
A doctor performs a physical exam as well as a neurological exam to determine if the stroke is affecting the nervous system. You will also receive several blood tests. Imaging tests, such as a CT scan and an MRI are performed, usually very quickly.
A CT scan uses x-rays to create images of the brain. This test can determine bleeding in the brain, an ischemic stroke, a tumor or other conditions. An MRI can detect brain tissue damaged by an ischemic stroke and brain hemorrhages.
Other, more precise, imaging tests include a carotid ultrasound and an echocardiogram. A carotid ultrasound uses sound waves to create images of the inside of the carotid arteries in the neck.
This test can detect plaque and deposits that may be hindering blood flow to the brain. An echocardiogram also uses sound waves to create images. In this case, the test looks more closely at the heart muscle to see if it can detect a source of clots that may have traveled to the brain.
Treatment
Treatment for this condition depends on whether it is the ischemic or hemorrhagic type. If you think you are having a stroke, it is vital to call 911 or your local emergency department immediately.
Ischemic
An ischemic stroke occurs when a clot or other obstacle occurs in a blood vessel that supplies blood to the brain. The treatments involve attempting to restore this flow.
This is usually first done with emergency IV medication. The medication is made up of drugs designed to break up clots. Timing is very important in that this medication must be given as soon as possible after symptoms start, 3 hours or earlier.
The gold standard treatment is an IV treatment called recombinant tissue plasminogen activator (TPA). This medication dissolves clots and restores blood flow to the brain. Your doctor will consider potential side effects, such as bleeding to the brain, before administration.
The sooner the medication is administered, the better the survival and recovery potentials.
Another way to treat this condition is through emergency endovascular procedures in which the clot is removed from inside of the blood vessel. Like IV medications, this treatment must be performed as soon as possible. Treating the clot directly may result in better outcomes and less long term disability than the IV medications. This procedure can be performed in two ways:
- TPA is delivered directly to the brain: Doctors insert a long, thin tube through an artery in the groin and into the brain, where the medicine can be delivered directly to where the stroke is happening.
- The clot is removed: Doctors use the same catheter approach as delivering TPA except that a device is attached to the end, which is used to remove the clot. This procedure tends to work better for patients with large clots that are difficult to dissolve with TPA.
After the immediate danger has passed, your doctor may recommend additional procedures to prevent another stroke from occurring. These include removing plaques and/or opening the blood vessels with angioplasty and stents.
Hemorrhagic
This type of the condition is caused by bleeding in the brain. Treatments are designed to control the bleeding and reduce pressure on the brain.
Medications: If you are taking blood thinners, doctors may immediately give you medications that counteract this effect. There are also certain medications that will lower pressure in the brain.
Surgery: A surgeon can remove the excess blood and relieve pressure on the brain. Additional surgery options can be used to prevent a recurrence. A tiny clamp may also be inserted at the site of aneurysm to stop blood flow.
A coiling (endovascular embolization) is another surgical procedure in which a doctor inserts a catheter through an artery in the groin to the brain. Tiny detachable coils fill the aneurysm and force the blood to clot.
If you liked this article, you should check out our other posts in the Nebula Research Library!
Other public sites to reference when investigating strokes are the American Heart Association and American Stroke Association.
July 18, 2023