Nebula Genomics DNA Report for IBS
Is IBS genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

Table of contents
Is IBS Genetic?
There is no simple or direct answer to this question. This is because while genes can contribute to IBS development, they can also be developed without genetic grounding.
Genetics depicts the sequence of the DNA on a chromosome. There is also a term known as epigenetic that describes how behaviors affect genes. This means that an individual can possess behavior that can switch on or off a gene that causes certain conditions.
Experts see IBS in family histories, indicating that it is heritable and even possibly genetic. However, it is often difficult to determine if the disease presence is caused by heritable genes or a product of the family having similar behaviors and lifestyles, especially when it comes to diet and stress.
Research
Research published in 2016 by study authors Maria Henström and Mauro D’Amato explored the genetic risk of developing IBS. The condition is found to have stemmed from polygenes. Polygenes are genes with individual effects too small to make a noticeable difference, but that can produce a noticeable variation in combination with others. This means that they can be very significant when it comes to causing digestive problems.
In a few cases, diseases like IBS may result from single-gene mutation. The most convincing genetic variant in the 2016 paper was the TNFSF15 gene, which was also successfully replicated in independent cohorts.
Genetics that affect other parts of the body may have an indirect effect on the condition, such as the brain gut interactions. For example, a paper published in 2014 found that about 2% of patients with the condition carry mutations in SCN5A (which encodes the nav1.5 channel), which leads to loss of function of a sodium channel. If these two physiological conditions can be linked, more treatment options are possible.
A paper published in 2021 used a genome wide association study of 53,400 people demonstrated that the condition could be linked to mental health conditions such as anxiety and depression.
Introduction
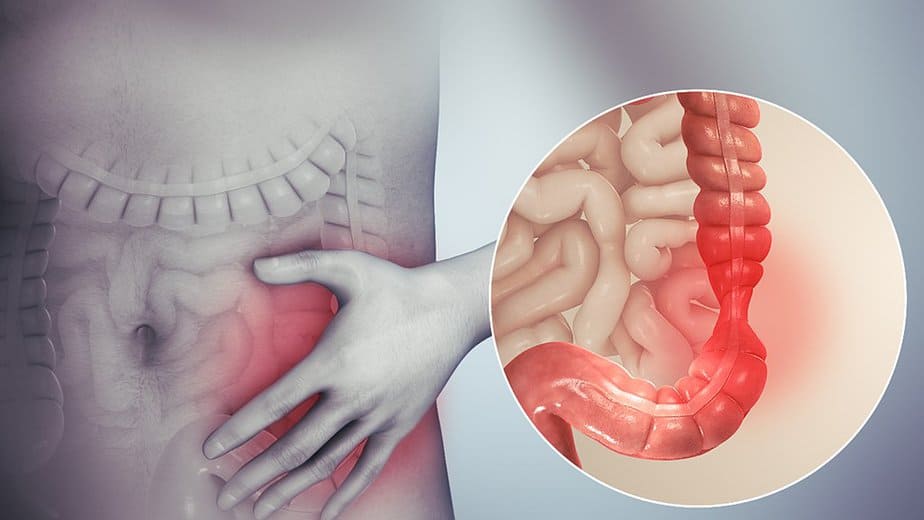
Irritable bowel syndrome (IBS) is a common disorder of the gastrointestinal tract that often causes stomach discomfort including cramping, abdominal pain, bloating, gas, and diarrhea or constipation, or both.
This condition is a long term condition that requires lifelong management.
Irritable Bowel Syndrome also goes by various other names. If you are suffering from the condition you may hear names such as:
- Irritable colon
- Spastic colon
- Irritable bowel
- Nervous stomach

Patients face issues such as abdominal pain and cramping that can occur over a long period. These symptoms can cause oversensitivity of the gastrointestinal tract, further causing unusual contraction of the bowels. The result of this unusual contraction can be constipation, abdominal pain, and diarrhea.
The disorder affects the gut-brain interaction, causing a shift that results in serious discomfort to sufferers. There are different types, categorized based on individual bowel movements. It’s important to note that some medications and treatments only work for specific types.
It often takes a long time to detect IBS. This happens because in most cases inconsistent bowel movements are not a cause for concern. This makes it seem like a negligible defect in the digestive tract until worse symptoms occur.
Types
The various types include:
Diarrhea predominant IBS or IBS-D: Characterized by loose and watery stool.
Constipation predominant IBS or IBS-C: Characterized by hard and lumpy stool.
IBS with Mixed Bowel Habits or IBS-M: A combination of IBS-D and IBS-C.
People with IBS tend to have irregular, uneven contractions compared to those without the disorder. This unusual movement causes pain and cramps. Some of the symptoms can be due to excess bacteria growth in the GI tract.
Due to their similar presentations, the symptoms of IBS and colon cancer are often similar. However, because the former does not cause damage to the GI tract its presence does not increase the likelihood of the cancer.
There is some evidence to suggest that IBS is a disease of industrialization and urbanization. Studies supporting this idea cite higher stress and a western diet as contributing factors that promote the symptoms in those of higher socioeconomic class. This could also explain why rates are rising in areas in Asia, South America, and Africa where affluence is rising.
Inflammatory Bowel Disease
IBS should not be confused with inflammatory bowel disease (IBD). IBD is classified as a disease as opposed to a syndrome. Although it has similar symptoms, it leads to chronic inflammation and damage to the GI tract that doctors can diagnose via imaging. It can lead to other problems such as colon cancer.
Epidemiology
The prevalence of this condition varies with location and age. Worldwide, experts believe it to be between 10% and 25% with an average of 11.6%. These figures vary greatly depending on the country with the highest burden being present in Europe, Southeast Asia, and North America. In the United States, IBS affects between 25 and 45 million people.
The condition is more common in women in almost all populations with women being diagnosed at 1.5- to 3-fold higher rates than men. It can occur at any age, including in children. Most patients report symptoms by age 35 and it is less likely they will be diagnosed over 50 years of age.
Symptoms
The major focus of this functional gastrointestinal disorder is the digestive system or the GI tract. The most common symptom of the condition is abdominal pain that affects quality of life. Doctors also link it with frequent constipation and or diarrhea. People who suffer from the disorder usually also experience a shift in bowel habits.
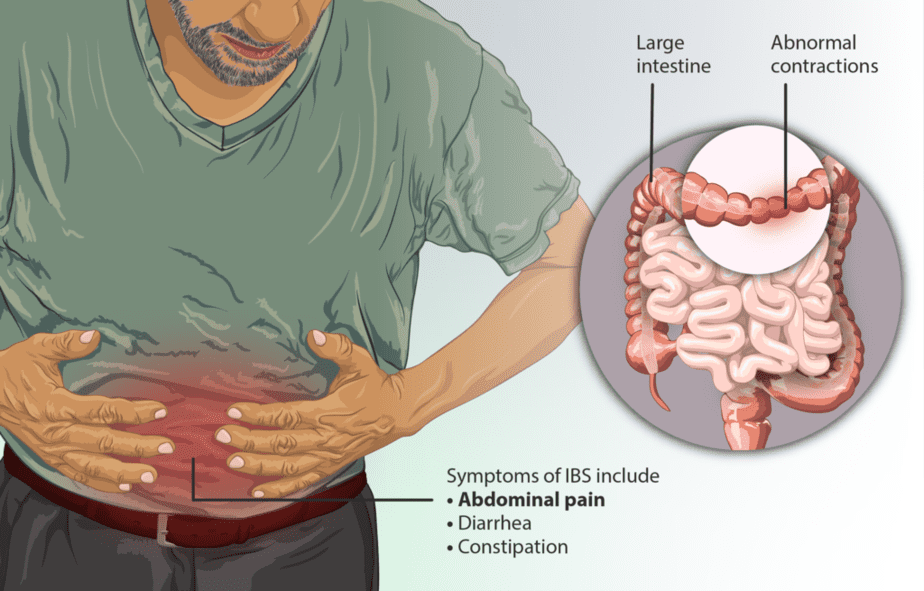
https://www.myupchar.com/en via Wikipedia Commons. CC-Attribution-Share Alike 4.0 International.
One major issue associated with this condition is that attacks may be acute, occurring and subsiding within a day. A sign that irregularity may be something more is when the problem occurs recurrently. There may also be the feeling of bloating or incomplete evacuation.
Other symptoms include:
- Gastroesophageal reflux
- Fibromyalgia
- Headache
- Backache
- Depression
- Anxiety
- Sexual dysfunction
- Low libido
Contrary to popular belief the condition does not cause weight loss. Any unexpected changes in weight may be due to stress or treatment.
Causes of IBS
Although there are specific things that contribute to IBS, including genetic and environmental factors, it is difficult to point out the main cause.
If you have issues with how your GI muscles contract to move food, sensitive nerves in the GI tract, or issues with brain-gut communication, the risk of developing IBS increases. Triggers don’t necessarily cause the disorder but can lead to acute attacks. Factors that trigger this disorder are emotional stress and certain foods and medications.
Although experts have not proven depression and anxiety cause the disorder, these conditions worsen the situation. Antibiotics could raise the risk of suffering from the condition. Research also shows that defects in genetic innate immunity and homeostasis can increase the risk of IBS.
Stress is another risk factor that plays a role. Studies have been shown that IBS is associated with children who suffer physical and psychological abuse. Stress spikes up the development of the disorder in predisposed individuals. This is why people with stress issues or anxiety tend to have worse situations when they have IBS.
Another factor that can increase the risk of this disorder is a lack of a good diet. People with IBS are mostly known to be deficient in diets containing vitamin D. Quality content of vitamin D helps to regulate the immune response, gut microbiome, and inflammatory processes that can increase the risk of IBS.
Overgrowth of bacteria in the intestine can also increase the risk of the disorder. Small intestine bacterial overgrowth (SIBO) is higher in individuals who are diagnosed with IBS. Increased bacteria growth is common in people with diarrhea-predominant IBS.
Diagnosis
Currently, there is no specific laboratory or imaging test to detect IBS. Instead, doctors will diagnose IBS based on your symptoms. It is important to state that care should be taken as some of these symptoms could be signs of other health issues not related to the condition, such as celiac disease. Because of this health care professionals will take a full medical history and other analyses such as blood tests to rule out other conditions.
If your doctor suspects IBS they will usually use the Rome criteria to confirm the diagnosis. The criteria allow the investigation to be solely based on the symptoms suffered by the patients.
Rome criteria
The Rome criteria states that patients must have recurrent abdominal pain at least one day per week in the last three months associated with:
- Change in recurrence of stool
- Change in the appearance of stool
- Defecation
If a doctor determines that the condition is present they will then diagnose the subset by asking the patient about stool form. The subset can be IBS-D (IBS with diarrhea), IBS-C (IBS with constipation), or IBS-M (mixed).
Treatment
Although there is no cure, several IBS treatments are effective in reducing the symptoms. Some of these measures include diet and lifestyle modifications, over-the-counter and prescription medications, and talk therapy to reduce stress.
Diet
Studies suggest that fibers such as psyllium, etc, are effective in managing IBS. It helps patients with IBS-D to pass out consistent stool. It also allows people with IBS-C to pass a moist stool.

Doctors may also recommend patients avoid triggering foods, drink fluids, and increase sleep and exercise. A dietician can often help patients with eliminating gluten or starting a FODMAP diet. This specialized diet requires avoiding and adding types of food, including certain fruits and vegetables.
Medication
Medications can also be useful in treating IBS. Some non-specific medications are effective at treating symptoms. These include over-the-counter medications such as fiber supplements, laxatives, anti-diarrheal, and pain medications. Antidepressants have also been found to be particularly effective for patients with pain and diarrhea as these medications work on the gut’s nervous system.
On the other hand, patients also have the option of prescription medicine designed specifically for the condition. Different therapies are prescribed for IBS-D and IBS-C.
Doctors treat IBS-D with loperamide, rifaximin (Xifaxan), eluxadoline (Viberzi), and alosetron (Lotronex) whereas they treat IBS-C with lubiprostone (Amitiza), linaclotide (Linzess), and plecanatide (Trulance).
Psychological therapy
Because stress appears to play a strong role in IBS systems, mental health treatment can be a way to find relief. A history of stress is often a precursor to IBS. People who have more symptoms of psychological stress like anxiety or depression tend to notice that IBS symptoms increase. Thus behavioral cognitive therapy for these conditions may have a secondary effect of reducing IBS.
You can learn more about IBS from the National Institute of Diabetes and Digestive and Kidney Diseases.
If you liked this article, you should check out our other posts in the Nebula Research Library!
February 24, 2023
