Table of contents
Nebula Genomics DNA Report for Scoliosis
Is scoliosis genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

What is Scoliosis?
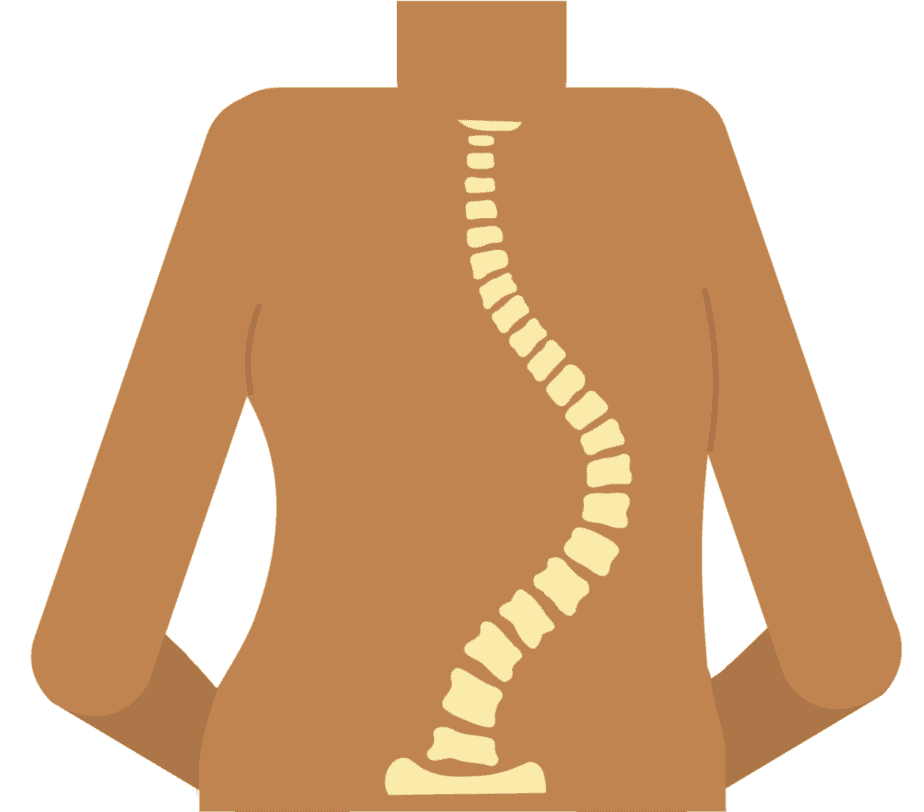
Scoliosis causes an abnormal S-shaped or C-shaped curve in the spine (spinal deformity). It can happen on either side of the spine and in different areas. Specifically, it is a lateral deviation of the spine from the longitudinal axis with rotation (twisting) of the vertebrae around the longitudinal axis and rotation of the vertebral bodies. Overall, this leads to structural deformations of the vertebral bodies.
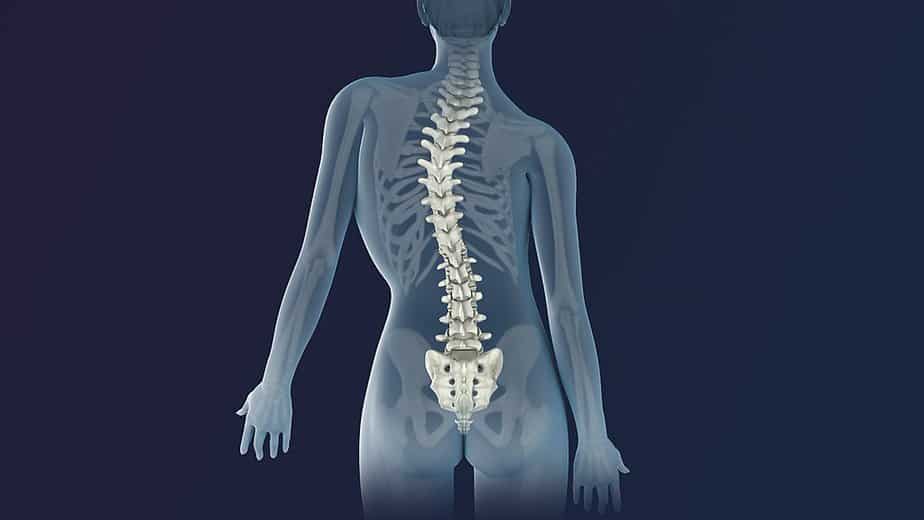
But the condition might not only make the spine deform to the left or right. The spine has three natural curves that help support movement and stress. Scoliosis progression may cause deformities on these too.
The onset of scoliosis normally occurs in late childhood or early teens (children ages 10-15 years old), during the growth spurt shortly before puberty. Most cases are mild, but others may get worse as children continue to grow. Some instances even become debilitating. Extreme scoliosis cases affect the amount of space in the chest, negatively affecting the function of the lungs.
With treatment and monitoring, children with the condition go on to lead healthy, active lives.
Classification
Scoliosis is classified according to the cause and time of origin, the curvature location and pattern, the extent (angles of curvature and degrees of rotation), and the curvature orientation (left, right). A form whose cause is unknown is called idiopathic scoliosis. About 90% of all cases are this type. In a small percentage of scoliosis patients (10%), when the cause is known, it is symptomatic or secondary scoliosis.
Some types of scoliosis include:
- Congenital: occurs when the spine does not develop fully in the womb
- Early-onset: occurs before puberty (between birth and age 10)
- Adolescent idiopathic (AIS): occurs when a child is growing. Spine curvatures and twisting occur at the same time
- Degenerative: occurs in older adults as bones age. This type usually occurs in the lumbar spine (lower spine)
- Neuromuscular: a curvature of the spine caused by a neurological or muscular condition such as cerebral palsy, muscular dystrophy, or spina bifida
- Scheuermann’s kyphosis: occurs when the front sections of the vertebrae (small bones that make up the spine) grow more slowly than the back sections during childhood
- Syndromic: spine curves as the result of a separate condition
Is Scoliosis Genetic?
Researchers suspect that several genetic factors may contribute to the development of scoliosis. Even more contribute to how severe the disorder is and whether the spinal curve progresses. Although many genetic variants have been mildly associated with scoliosis, very few have been clearly linked.
Is scoliosis hereditary?
According to OrthoInfo, about 30% of patients with adolescent idiopathic scoliosis have a family history, and first-degree relatives of patients have an 11 percent chance of developing it themselves. Additionally, genetic studies found patients with 14 or more of 28 genomic variants were 33% more likely to develop a severe form of scoliosis.
Current Research on Scoliosis
Through genetic research, scientists discovered that there is a genetic predisposition to scoliosis. This paper published in Nature Communications in 2019 uses a genome wide association study to identify 14 previously unknown genetic components of the condition.
Now, is scoliosis hereditary? It usually runs in families.
When a child has a family history, they will be examined. A child may be predisposed to develop the condition, but most of them do so slightly (mild scoliosis) and require no intervention.
This study, published in 2019, made a granular analysis between the type of scoliosis and the positive functional genomic groups. It discovered that most of the variant patterns for the condition had a rather low probability of developing any form.
As mentioned earlier, It is very common to find the curve during growth spurts. As a consequence, teenagers have a higher incidence, which is the reason why you can note a catalog of 133 studies on adolescent idiopathic scoliosis in clinicaltrials.gov. The PubMed database also has its share of a hundred studies on the same topic.
Speaking of growth sprouts, this thorough 2018-revised article provides guidelines for the rehabilitation treatment for scoliosis during growth. This cites several articles, including participants who are identical twins, demonstrating that genetics is only part of the story. This research reviews many of the options to correct adolescent idiopathic scoliosis (AIS).
If you are interested in the development of research for the condition from 2009 to 2018, you can take a look at these publication trends between those years.
Epidemiology
Scoliosis is a fairly common disease. In 2013, a literature review suggested there was anywhere from 0.47-5.2% prevalence of adolescent idiopathic scoliosis worldwide. Most sources average this out to be around 3%, especially in the United States.
Generally, the condition is more common in females than males. Additionally, you have a greater chance of developing the adolescent idiopathic form if you have a family member with this condition.
Scoliosis Symptoms
Scoliosis symptoms vary depending on the severity of the disorder. Common visible signs and symptoms of most scoliosis may include:
- Uneven shoulders
- One shoulder blade appears more prominent than the other
- Uneven waist
- One hip higher than the other
- Trouble breathing (more severe cases)
- Chest pain (rare)
If a scoliosis curve worsens, the spine will not only curve side to side but will also rotate or twist. This can be observed as ribs on one side of the body will stick out farther than on the other side.
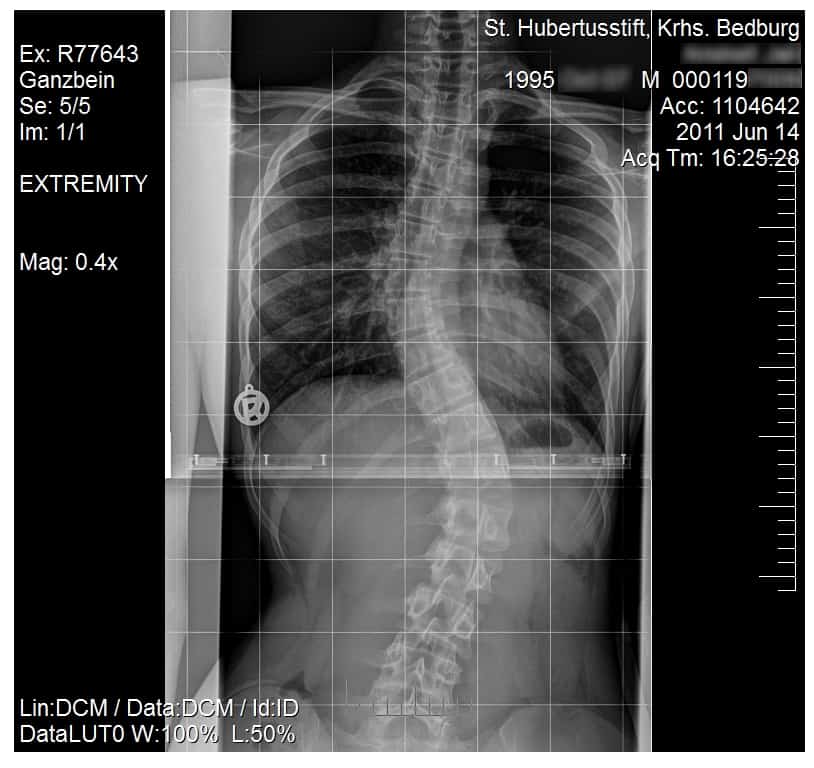
In the most severe cases, the rib cage may press against the heart and lungs, making it difficult to breathe and leading to heart disease. Young people who develop scoliosis are also at a higher risk of developing chronic back problems.
If the condition worsens so that physical signs are noticeable, it often negatively impacts self-esteem and mental wellbeing.
Scoliosis Causes
In a majority of cases (about 90%), the scoliosis causes are unknown. It is observed that it runs in families, suggesting a hereditary component. Genetic causes of scoliosis are currently being studied. Females are also more likely to develop the condition than males.
Onset is most likely to occur around the time of puberty when children tend to grow rapidly. Overall, it may result from genetic and environmental factors, although this is more likely true in later-onset forms of the disorder.
Some people wonder, “can you develop scoliosis?” In adult scoliosis, it develops when the facet joints and discs in the spine begin to deteriorate. It can equally affect children and adults. Sometimes, a child is born with it, and on other occasions, an adult develops it later in life.
Some conditions are identified as risk factors, including:
- Neuromuscular disorders such as cerebral palsy and muscular dystrophy
- Congenital disabilities that affect the spinal bones, such as spina bifida
- Spinal injuries or infections
Diagnosis
A physical exam is usually the first step to diagnose scoliosis, especially in young children. The doctor will observe a child standing straight, with arms at their sides. They can check for spine curvature and whether shoulders and hips are symmetrical.
They may then ask the child to stand and bend forward at the waist with arms hanging down. This test, sometimes called the Adam’s test, allows the doctor to determine if one side of the rib cage is more prominent than the other or if there is additional curvature in the upper and lower back.
An x-ray of the spine is normally the next step in the diagnosis procedure. These images will confirm the diagnosis and reveal the severity of the spinal curvature.
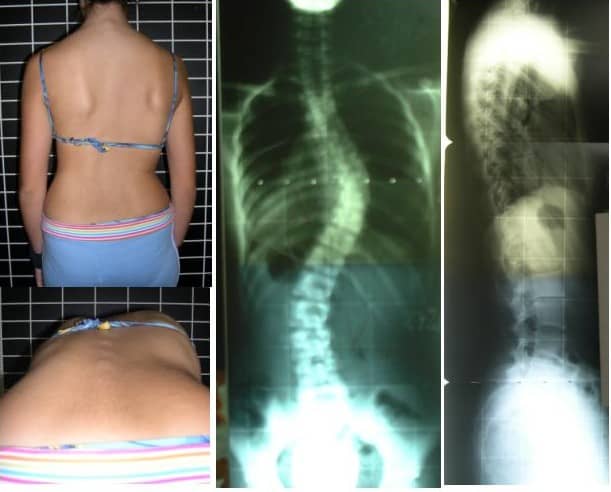
Other imaging tests are less common but may be recommended if another condition is also suspected. These additional tests may include MRIs, CT scans, and bone scans.
There is no genetic test for scoliosis but some variants may link to risks.
Treatment
Treatment options are very dependent on the individual and the progression of the disorder. Most children develop only a mild case of scoliosis, which does not require major treatment. If observed during puberty, children are normally monitored regularly to determine if the condition worsens over time. Doctors consider several factors when deciding on a more harsh treatment such as a brace or scoliosis surgery:
- Sex
- Severity of the curve
- Curve patterns (S curves tend to be more severe than C curves)
- Location of the curve (centered curves tend to worsen more often)
- Stage of bone growth (the condition does not usually progress in bones that have stopped growing)
Braces
Braces are most often recommended in children who are still growing and who exhibit a moderate form. Although a brace cannot fix the damage that has already occurred, it will stop the curve from getting worse. This is why braces are most effective in cases that are diagnosed early.
The most common type of brace is made of plastic and can fit easily under regular clothing. Most children are able to maintain their daily physical activities while wearing the brace. Its effectiveness is directly related to how often it is worn and why it is usually worn day and night. Once children stop growing, a brace will no longer be effective, so its use is discontinued.
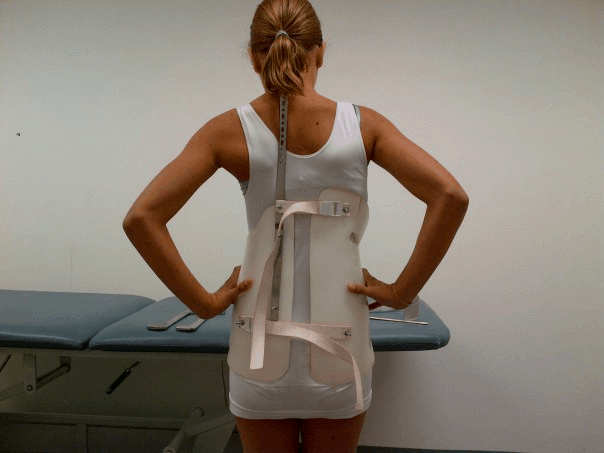
The American Association of Neurological Surgeons recommends braces for children still growing who have a curvature more than 25 to 40 degrees.
The Schroth Method
The Schroth Method is a form of physical therapy consisting of exercises specific for every case. The purpose of customizing the activities is to help the spine recover its natural position.
This non-surgical treatment option of treatment aims to help with posture, restore muscular symmetry, breathe into the concave portion of the body, and teach the patient how to be aware of their stance. To help with spaces in the vertebra that becomes compressed and with those that stretch, the therapy de-rotates, stabilizes, and elongates the spine in a three-dimensional plane.
Surgery
Severe scoliosis that is worsening with time may require a special type of surgery called spinal fusion surgery. Surgery is usually reserved for patients who have a curvature of over 40 degrees.
This type of surgery fuses two vertebrae so that they cannot move independently. The surgeon places bone grafts made of pieces of bone or a bone-like material between the vertebrae. Finally, metal rods, hooks, screws, or wires typically hold the spine straight while the old and new bone fuse.
If the child is still growing, an adjustable rod that can be lengthened as the child grows may be installed. All surgeries come with some risk of complications, including bleeding, infection, and nerve damage.
Prognosis
In mild to moderate cases, most people with scoliosis live full lives with few to no physical limitations. In more severe instances, people might find discomfort, pain, or mental distress.
Coping can be especially difficult for children and teens. Strong peer relationships and support groups may help with scoliosis in children who are having difficulty in managing. Support groups specifically for families affected by scoliosis may be instrumental in providing advice, resources, and connections with others who face similar challenges.
For more information on this condition in children and teens, you could reference the latest research from the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
If you liked this article, you should check out our other posts in the Nebula Research Library!
July 27, 2022