Table of contents
- Nebula Genomics DNA Report for Low Testosterone in Men
- What is Low Testosterone in Men? (Part 1 of Is low testosterone in men genetic?)
- Is Low Testosterone in Men Genetic?
- Current Research on Low Testosterone In Men [Updated June 2021]
- Epidemiology (Part 4 of Is low testosterone in men genetic?)
- Symptoms (Part 5 of Is low testosterone in men genetic?)
- Causes (Part 6 of Is low testosterone in men genetic?)
- Diagnosis (Part 7 of Is low testosterone in men genetic?)
- Treatment (Part 8 of Is low testosterone in men genetic?)
Nebula Genomics DNA Report for Low Testosterone in Men
Is low testosterone in men genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

| This information has been updated to reflect recent scientific research as of June 2021. |
What is Low Testosterone in Men? (Part 1 of Is low testosterone in men genetic?)
Testosterone is a sex hormone that occurs in all sexes but differs in concentration and mode of action in men and women.
In men, testes release testosterone largely as a reaction to LH (luteinizing hormone). This sex hormone is critical to the development of physical characteristics, like facial hair, muscle mass, formation of sex organs, sexual function, and a deeper voice, when a male child reaches puberty.

The adrenal cortex produces small amounts of other sex hormones but only a very small amount of testosterone. In women, the ovaries and adrenal cortex produce small amounts of testosterone, but normally not enough to trigger male characteristics.
Total testosterone is composed of 98% bound testosterone, either bioactive (albumin-bound) or sex hormone binding globulin (SHBG)-bound testosterone. The remaining 1 to 2% is free testosterone.
Hypogonadism is the medical term for diminished functional activity of the gonads (testes or ovaries). Low testosterone in men is often a result of lowered activity.
Is Low Testosterone in Men Genetic?
Low testosterone is, in most cases, a combination of age, lifestyle factors, and genetics. Previously, multiple genetic markers have been identified that are associated with decreased blood levels. The majority of these markers are located within the globulin gene. Globulin is a protein that binds to testosterone. Increased levels of the globulin protein could reduce testosterone in the blood.
Many of these genes can be found on the SHBG locus and on the X chromosome.
Other cases suggest that the condition is more likely driven by challenges in adolescence (such as poverty) than genetic destiny.
On the other hand, some genetic conditions result in low testosterone in men. Although these disorders affect the chromosomes, they are not hereditary. This means that they occur in the genes after conception and they are not passed through families.
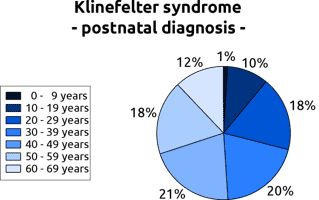
Klinefelter syndrome
Individuals with this condition have two or more X chromosomes in addition to a Y chromosome. This condition is not hereditary but occurs after conception. The result is abnormal development of the testes and thus low levels of testosterone. Persons with this condition usually also experience enlarged breasts, reduced body hair, lower body masses, and extremely low sperm count.
Kallmann syndrome
This condition is also linked to the X chromosome. LH and FSH hormones are impaired, decreasing the amount of testosterone that is produced. Although it can occur in both women and men, it is more common in the latter. In all cases, the individual may enter puberty late or not at all. Male testicles tend to be smaller and, as with Klinefelter syndrome, often leads to infertility.
Myotonic dystrophy
This is the most common form of adult muscular dystrophy. This genetic mutation is on the Y chromosome and is usually discovered when a person is in their 30s or 40s after testicular failure.
Current Research on Low Testosterone In Men [Updated June 2021]
Generally, it is believed that natural aging has the greatest influence on the health of humans. It’s true in most cases that low testosterone is caused by advanced age. However, there are also cases due to several other factors that range from genetics to health conditions. In addition, individuals with low levels are prone to a few health issues.
A study in 2017 evaluates the effects of testosterone deficiency on human health. In this study, it was found that a lower level could decrease the level of hemoglobin in the blood. The decrease in the level of hemoglobin usually results in mild anemia (low blood cell count).
Although there are treatments for deficiency, the treatment of age-related low testosterone levels should be considered carefully. Certain guidelines regarding this issue were published in 2018 by the American College Of Physicians.
These recommendations include the benefits, harms, and costs of treating age-related testosterone deficiency. The benefits that come from this treatment include an improvement to the quality of life and erectile and cognitive functions. However, this treatment also involves risk of pulmonary embolism, prostate cancer, adverse cardiovascular events, and mortality.
Thus, the authors recommend that clinicians discuss the risks and benefits with their patients and potentially discontinue any treatment within 12 months if the condition does not improve. They also recommend intramuscular treatment over transdermal treatment due to cost benefits. They do not recommend any treatment to improve certain attributes such as energy levels, vitality, physical function, or cognition.
There are also cases where exercises are the primary cause of low testosterone levels. This is majorly seen in athletes involved in a high level of endurance exercises. This is also referred to as Exercise-hypogonadal Male Condition (EHMC).
A study of EHMC in 2018 recommends clomiphene citrate as treatment due to its effectiveness. However, it is considered a banned substance and is not advisable if you participate in sports coordinated by the World Anti-doping Agency.
Generally, it would be best to treat EHMC as an athlete by regulating your exercises and by nutritional intervention. Furthermore, unless the deficiency of testosterone is accompanied by the symptoms of hypogonadism, it does not warrant treatment.
Epidemiology (Part 4 of Is low testosterone in men genetic?)
It is difficult to define low testosterone levels since the levels tend to vary throughout the day and may be affected by lifestyle factors such as weight, nutrition, alcohol consumption, and certain medications.
This condition can happen to men at any age, but it is much more prevalent in older males. Some estimates suggest that it affects over 40% of men aged 45 and older.
According to the Boston University School of Medicine, low testosterone affects an estimated 4 to 5 million men in the United States. More than 60% of men over age 65 have free testosterone levels below the normal values of men aged 30 to 35.
Symptoms (Part 5 of Is low testosterone in men genetic?)
While the medical term for low testosterone levels is hypogonadism, the condition is also referred to as Testosterone Deficiency Syndrome (TD) or Low Testosterone (Low-T). Some common symptoms in men include:
- Erectile dysfunction, or problems maintaining or developing an erection
- Other erection changes, such as fewer spontaneous erections
- Decreased libido or sex drive
- Infertility
- Rapid hair loss
- Reduced muscle mass
- Increased body fat
- Enlarged breasts
- Sleep disturbances such as sleep apnea
- Persistent fatigue
- Brain fog
- Depression
- Lowered bone density (especially in men over 70)
There are controversial opinions as to the link between low testosterone and prostate cancer. While some studies seem to show that increasing testosterone through supplements improves prognosis, others suggest that supressing the hormone may ultimately help reduce fueling cancerous prostate cells. The American Cancer Society indicates the latter approach on their website. This connection continues to be an active area of research.
Causes (Part 6 of Is low testosterone in men genetic?)
The most significant cause of low testosterone in men is age. It is believed that testosterone levels peak in adolescence and early adulthood and begin to decline by about 1% per year starting around age 30.
Younger men may also experience low testosterone. In these cases, increased risk of the condition is more likely to be comorbid with a different underlying disorder or the result of a separate illness or injury.
According to Healthline, some contributing factors include:
- High cholesterol levels
- High blood pressure
- Being overweight or obese
- Drinking excessive amounts of alcohol
- Using illegal drugs
- Using anabolic steroids
- Taking certain prescription medications such as steroids and opiates, especially in excess
Other medical conditions that may accompany or cause low levels:
- Hypothalamic or pituitary disease or tumors
- Injuries, tumors, or other conditions affecting your testicles including inflammation related to childhood mumps
- Inherited diseases, such as Kallman’s syndrome, Prader-Willi syndrome, Klinefelter syndrome, or Down syndrome
- Type 2 diabetes, heart disease, liver disease, or AIDS
- Cancer treatments such as radiation and chemotherapy
Diagnosis (Part 7 of Is low testosterone in men genetic?)
The condition can be diagnosed around puberty, which is ideal so that treatment can begin early. However, many men are unaware of their low testosterone levels until later in adulthood. As a result, many males are diagnosed when they realize they have fertility problems.
It’s important to seek medical advice if you think you have this condition so that you can be prescribed testosterone medication. Your health care provider may conduct a physical exam and ask questions regarding the development of characteristics such as pubic hair, muscle mass, and size of testes.
Testosterone levels are measured via a standard blood test that looks for one or more types of testosterone in the blood. Because levels tend to fluctuate throughout the day and may be affected by lifestyle choices, such as alcohol consumption, it is difficult to get the full picture with just one test. In most cases, your doctor will order a few blood tests on different dates to help diagnose low testosterone in males. The highest levels tend to be around early morning, which is why many of these tests are done before 10 am.
If low testosterone in men is observed through the blood test, you may be given additional tests to rule out or confirm a testicular disorder of pituitary gland abnormality. These tests include:
- Hormone testing
- Semen analysis
- Pituitary imaging
- Genetic studies
- Testicular biopsy
Did you know you can test for low testosterone in men at home at a fraction of the cost? Learn more in our article about at home testosterone tests.
Treatment (Part 8 of Is low testosterone in men genetic?)
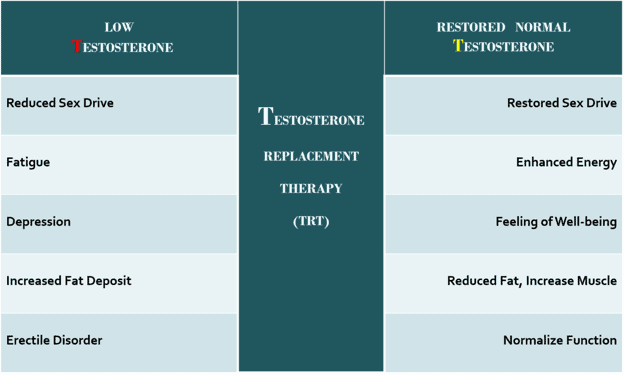
According to Mayo Clinic, low testosterone treatment in men depends on the age of diagnosis and the cause of the low levels. For most adults, the condition is treated with testosterone replacement therapy. This type of hormone replacement therapy is generally provided to young men who wish to increase the characteristics the condition takes away, such as sexual drive, facial hair, and muscle mass.
Adults
There are many different testosterone products that vary in how they are administered. Most need to be taken for a long term. Some are more convenient than others, which may influence you and your doctor’s decision.
Oral: Oral testosterone replacement therapies are generally not prescribed mainly due to side effects damaging the liver. A new oral treatment, testosterone undecanoate (Jatenzo), was approved by the FDA in 2019. This preparation is absorbed by the lymph nodes, allowing it to bypass the liver.
Gel: Depending on the brand, gels are applied either to the upper arm/shoulder or front/inner thigh. The medicine is absorbed through the skin, so it is important not to wash the gel off for several hours. Skin irritation may occur. It is also important to avoid inadvertently transferring the medication to another person through skin-to-skin contact.

Injections: Testosterone cypionate (Depo-Testosterone) and testosterone enanthate are injections given in a muscle or under the skin. They can normally be given at home by either yourself or a family member. An alternative is testosterone undecanoate (Aveed). This is a deep intramuscular injection that is typically given every ten weeks. It must be taken at your doctor’s office and can have serious side effects.
Patch: There is a testosterone-containing patch (Androderm) available that is applied on either the thigh or torso. Mild side effects, such as skin irritation, may occur.
Gum and cheek (buccal cavity): This is a small putty-like substance applied to the gumline three times a day. The testosterone replacement is absorbed into your bloodstream where your gum meets your upper lip. Gum irritation may occur.
Nasal: This testosterone gel (Natesto) can be applied to the nostrils. It is pumped into each nostril twice, three times a day. Depending on your daily routine, it may be more inconvenient than other options.
Implantable pellets: Testosterone-containing pellets (Testopel) can be surgically implanted under the skin every three to six months.
Infertility
Depending on the cause of low testosterone, there may be treatments to restore fertility. If a pituitary problem is the cause, pituitary hormones can be prescribed to stimulate sperm production and fertility. Pituitary tumors can be either surgically removed or treated with chemotherapy or radiation.
In most other cases where fertility cannot be restored, there are technological options that can help couples conceive.
Children
If a boy is experiencing delayed puberty, it may be possible to induce it with hormonal supplements. Three to six months of testosterone supplementation given as an injection is usually recommended. After this time, the child normally develops the traditional male characteristics such as facial hair and muscle mass.
If you liked this article, you should check out our other posts in the Nebula Research Library!
