Table of contents
Nebula Genomics DNA Report for Prostate Cancer
Is prostate cancer genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

What is Prostate cancer?
Prostate cancer is a cancer of the prostate, a gland in the male reproductive system that produces some of the fluids contained in seaman, the liquid that carries the sperm. The prostate is located around the urethra, just below the bladder.
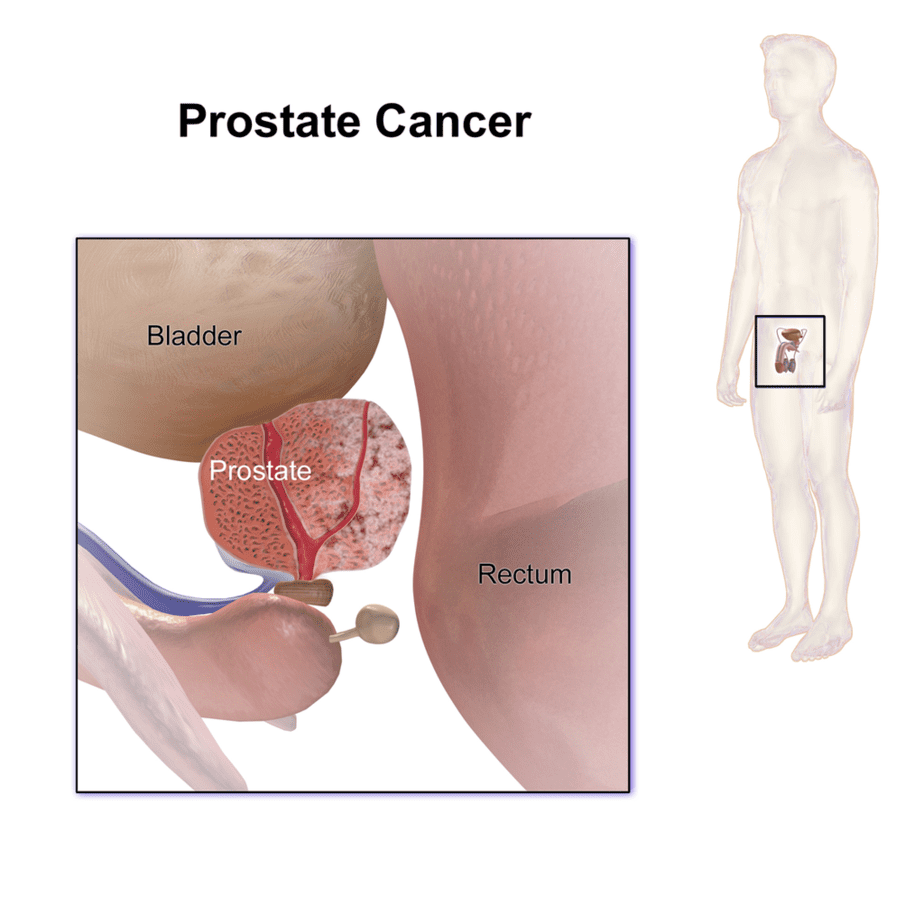
Most of these forms of prostate cancers grow slowly and some patients may not realize it is present for years if it does not cause symptoms. Later signs often include pain or difficulty urinating, blood in the urine, or pain in the pelvis or back.
Older age and having family members with the condition are the most important risk factors for this cancer, with most diagnoses of prostate cancer occurring over age 50. There are also some genetic factors that may lead to the disease. A doctor uses a biopsy to perform the initial diagnosis.
In most cases, detecting cancers early is crucial for helping patients live longer. However, sometimes, treatment for this condition is not necessary and doctors will instead use the practice of watchful waiting. This is when a doctor avoids treatment as the five year survival rate is very high. If a doctor decides that treatment is necessary, they will most often recommend surgery, radiation therapy, hormone therapy, or chemotherapy either alone or in combination.
Is Prostate Cancer Genetic?
There is some evidence from cancer research that inherited mutations may lead to an increased prostate cancer risk. Overall, experts believe that about 10% of cases are associated with hereditary prostate cancers. Inheriting many multiple of these mutations may lead to a significant genetic-based increased risk of prostate cancer.
BRCA1 and BRCA2 genes: These are the most common inherited mutations in other cancer types such as breast cancer and ovarian cancer. It can also increase the chance of getting prostate cancer in males. They are tumor suppressor genes that help repair DNA damage or cause cells to die.
HOXB13: This gene codes for a protein that helps regulate other genes. Experts believe it acts as a tumor suppressor gene.
CHEK2, ATM, PALB2, and RAD51D: These are DNA repair genes.
RNASEL (formerly HPC1): This tumor suppressor gene helps cells die when needed.
Men with Lynch syndrome, an inheritied condition, also have an increased risk for a number of cancers, including colorecterol and prostate cancer. The genes affected are those associated with DNA repair when the cell is preparing to divide.
If you have a father or brother with prostate cancer your doctor may recommend more frequent screening or prevention measures.
Genetic counselors may be able to provide additional information in coordination with genetic testing and genetic counseling sessions. Learn more about genetic testing for prostate cancer!
Epidemiology
According to the American Cancer Society, prostate cancer is the second most common type of cancer among men. Skin cancer is the most common cancer among men. About 1 in 8 men will be diagnosed with prostate cancer during his lifetime. In 2021, there were about 250,000 new cases of prostate cancer.
Men with prostate cancer tend to be older, with the average age of diagnosis being 66 and very few cases detected in men less than 40. It is more common in non-Hispanic men of African ancestry. Because of this, it is especially important for African American men to check with their doctor about screening and prevention.
It is the second leading cause of death from cancer in men after lung cancer with about 1 in 41 men dying from prostate cancer. However, most men who are diagnosed will not die from the disease. In 2021, more than 3.1 million men in the United States are living with a prostate cancer diagnosis.
Symptoms
In some cases prostate cancer starts with no symptoms of the disease for years. However, if you notice any of the following signs, you should consult with a medical professional to determine if the symptoms are a result of prostate cancer or other conditions:
- Difficulty starting urination
- Weak or interrupted flow of urine
- Difficulty emptying the bladder completely
- Frequent urination
- Urge to urinate frequently at night
- Pain or burning during urination (less common)
- Blood in the urine or semen
- Painful ejaculation
Some signs that the aggressive prostate cancer may have spread to other areas of the body, including nearby seminal vesicles, rectum, bladder, or pelvic wall, include:
- Pain in the back, hips, or pelvis that doesn’t go away
- Swelling or fluid buildup in the legs or feet
- Unexplained weight loss
- Fatigue
- Change in bowel habits
Other, noncancerous conditions, such as an enlarged prostate, may cause similar symptoms. They may also be associated with things unrelated to cancer like a bladder infection.
Causes
As with all cancers, changes in the DNA that allow prostate cells to grow too quickly cause the disease. These changes are either in oncogenes, which help cells grow and divide or tumor suppressor genes, which keep cell growth under control.
When genetic mutations cause oncogenes to remain on or tumor suppressor genes to remain off, there is a greater chance that the cells will grow out of control, resulting in prostate cancer.
Some genetic mutations are acquired, or picked up through a person’s lifetime. Parents do not pass these mutations to their children. There are several risk factors that increase that chance of developing prostate cancer that can lead to acquired mutations.
Patients can control some of these mutations to an extent through lifestyle choices but not others. Experts believe that patients acquire most genetic variations associated with prostate cancer. These risk factors for prostate cancer include:
Age: The chance of being diagnosed increases rapidly after age 50
Race: The disease is more common in non-Hispanic Black males
Geography: It is most common in North America, northwestern Europe, Australia, and on Caribbean islands. It is less common in Asia, Africa, Central America, and South America. Experts believe this in an effect of more screening and western diets.
Family history of prostate cancer: The condition appears to run in families. Having a father or brother with the disease doubles an individual’s risk of developing prostate cancer as well. Having family members on the same side of the family also increases risk.
Some other factors that may contribute to high risk include a high fat diet, obesity, smoking, chemical exposures, inflammation of the prostate gland, sexually transmitted infections, and having a vasectomy.
Diagnosis
Although screening for prostate cancer is an option, doctors generally do not recommend early screening for younger men with no history of the disease. Men over 50 should discuss screening options with their health care professional. They usually decide on screening based on patient risk factors and potential benefit of early detection.
Screening options include:
Digital rectal exam (DRE): During this test, a doctor inserts a gloved, lubricated finger into your rectum to examine the prostate. They will usually be able to detect abnormalities in the texture, shape or size of the gland.
Prostate-specific antigen (PSA) test: This PSA blood test looks for a substance that’s naturally produced by your prostate gland. Higher than expected levels in the blood may indicate prostate infection, inflammation, enlargement or cancer.
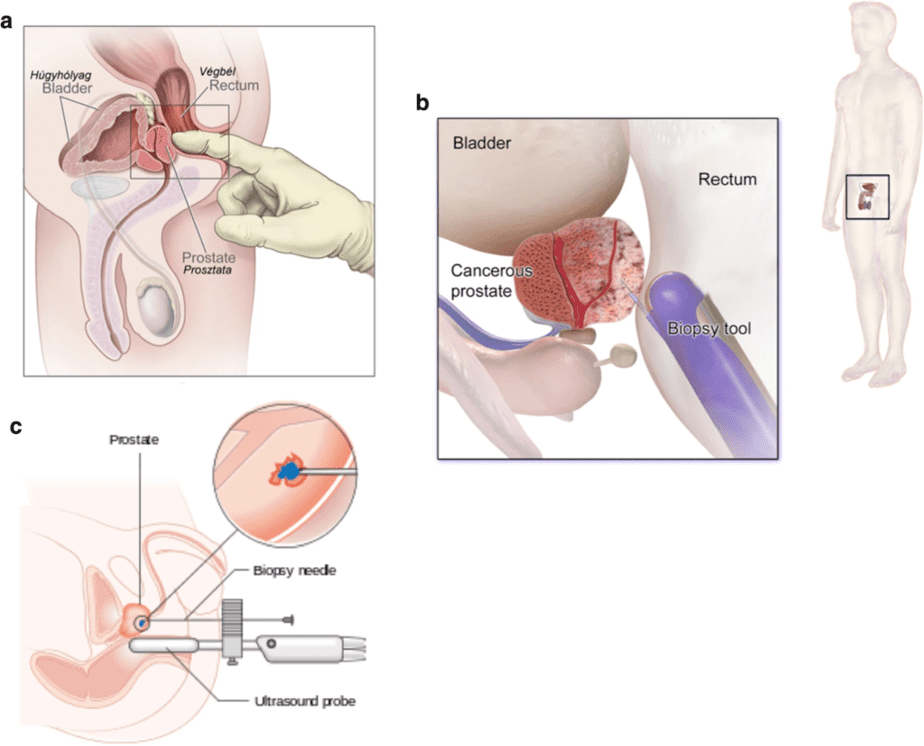
Screening may suggest the presence of cancer, but official diagnosis must be performed using other methods:
Ultrasound: This imaging technique uses a small probe inserted in the rectum to visualize the prostate gland.
Magnetic resonance imaging (MRI): An MRI can provide a more detailed image of the prostate.
Biopsy: This procedure involves collecting a small sample of cells from the prostate, from which your doctor can determine whether cancer cells present. A prostate biopsy is often done using a thin needle that’s inserted into the prostate to collect tissue.
Other imaging procedures such as bone scans, ultrasounds, CT scans, MRIs, and PET scans can help determine if the cancer has spread. Depending on the extent and aggressiveness of the cancer, your doctor will assign a stage of I through IV. Stage I cancer indicates that it is localized to the prostate while Stage IV indicates it has spread to other areas of the body. This stage may also lead to other conditions, such as pancreatic cancer.
Treatment
Doctors recommend treatment for prostate cancer based on the type, whether it is an aggressive, and overall patient health.
Watchful waiting
Doctors typically recommend active surveillance when the cancer is localized, not growing fast, and not causing symptoms. They use regular follow-up blood tests, rectal exams and prostate biopsies to monitor the progression of the cancer. If the cancer starts progressing, they may recommend additional treatment. Doctors may also recommend this process for advanced cases in which treatment is difficult.
Surgery and radiation
Surgery involves removal of the prostate gland along with some surrounding tissues (radical prostatectomy). Doctors recommend this treatment for cancer localized to the prostate or high grade cases. The surgeon may perform this procedure by using a mechanical robot to control several small incisions in the abdomen.
This is the most common technique. In some cases, the surgeon may make one long incision although this is much more rare.
Radiation uses high-powered energy to kill cancer cells. A patient has two different options.
First, doctors can apply the radiation to the prostate cancer from the outside of the body. Treatments usually occur for five days a week for several weeks.
They can shorten this time by applying higher energy for shorter time periods. Doctors usually recommended this method for treating cancer in the prostate or after surgery to kill any remaining cancer cells. They can also use it to treat the condition if it has spread to other parts of the body,
The second method is brachytherapy, in which radiation is applied from inside of the body. Doctors perform this procedure by placing rice-sized radioactive seeds in the prostate tissue. This allows for a lower dose of radiation for a longer period of time. It is most appropriate for cancer that has not spread.
In some cases, doctors use both types of radiation in combination.
Freezing or heating therapy
Applying high heat or cold directly to the prostate can help kill cancer cells. Doctors usually use these procedures if the cancer is small and would make surgery difficult. They may also be used if patients have not had success with radiation.
Hormone therapy and chemotherapy
Prostate cells need the hormone testosterone to grow and divide. By using hormone treatment to prevent testosterone from reaching the prostate, doctors can force the cancer to slow or die.
Medications can stop your body from producing testosterone or block testosterone from reaching the prostate. Surgerions may also remove the testicles, which significantly decreases the testosterone in the body. Doctors often use hormone therapy to treat advanced prostate cancer to shrink the cancer and slow its growth.
Chemotherapy uses medications to kill rapidly growing cells. This option is usually for patients for which the cancer has spread to other parts of the body.
There is no way that prostate cancer can be prevented, but you can take steps to reduce your risk through a healthy diet and exercise.
Finally, new treatments including immunotherapy and targeted drug therapy, may also have advantages in treating this condition.
If you liked this article, you should check out our other posts in the Nebula Research Library!
January 26, 2023
