Table of contents
Nebula Genomics DNA Report for Blood Cancer
What is blood cancer and is it genetic? We created a DNA report based on a study that attempted to answer this question. This article covers all blood cancers while the report focuses on the specific type, extranodal natural killer T-cell lymphoma. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

| This information has been updated to reflect recent scientific research as of August 2021. |
What is Blood Cancer?
Blood cancer is a generic term for a class of cancers that affect blood and bone marrow (spongy tissue inside of bones where blood cells are made). Although there are three different types of blood cells in the body, blood cancers only affect white blood cells. These cells are an essential part of the immune system that help the body fight off infection. This type of cancer tends to cause the body to produce white blood cells that do not function properly. When too many poorly performing white blood cells are present, a patient experiences the signs and symptoms of the condition.
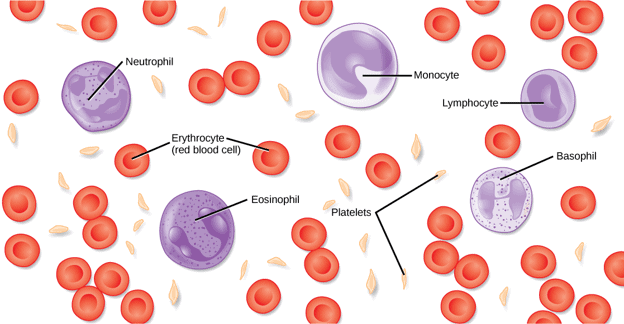
The other types of blood cells -red blood cells and platelets-are not directly affected.
Types of Blood Cancer
There are 3 types of blood cancer: leukemia, lymphoma, and myeloma. Signs and symptoms often depend on the type of cancer.
Leukemia blood cancer
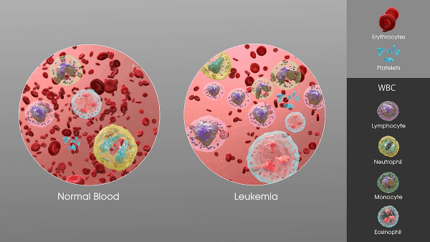
Leukemia occurs when the bone marrow makes too many abnormal white blood cells and the leukemia cells interfer with the production of red blood cells and platelets. There are four main types of leukemia called acute lymphocytic leukemia (ALL), acute myeloid leukemia (AML), chronic lymphocytic leukemia (CLL), and chronic myeloid leukemia (CML). Types labeled as acute mean that the cancer progresses quickly, while those labeled chronic mean that it progresses more slowly.
Acute
Patients with ALL make too many lymphocytes, a type of immature white blood cell, that crowd out the mature, healthy blood cells. This is the most common cancer in children, and the prognosis is generally very good. ALL can also occur in adults over 50.
AML is also an acute, or rapidly progressing disease. However, this type starts in the myeloid cells, which can grow into any of the blood cell types (red blood cells, white blood cells, and platelets). Having this cancer lowers the amount of all of these blood cells. This type of cancer typically affects patients who are 65 and older and is more common in men than in women. Smoking is the only lifestyle factor associated with an increased chance of developing this blood cancer.
In both cases, previous cancer treatments, including radiation therapy, other radiation exposure, and certain genetic disorders, such as Down syndrome, increase your risk.
Chronic
CLL is the most common type of blood cancer in adults, usually affecting those over 70. Like ALL, this disease starts in the lymphocytes. However, unlike ALL, it tends to progress slowly. As a result, some patients are diagnosed until years after the cancer starts. The disease is slightly more common in males and is more common in North America and Europe than in Asia.
CML is the least common form of leukemia. Although it can occur at any age, the risk of developing leukemia increases for older adults. Like AML, it starts by affecting the myeloid cells in the bone marrow. Like CLL, this blood cancer affects males more than females.
In both cases of chronic leukemia, exposure to radiation increases your chances of developing this condition.
Lymphoma blood cancer
This type is classified as either non-Hodgkin lymphoma or Hodgkin lymphoma. In both cases, the cancer originates in the lymphatic system and causes white blood cells called lymphocytes to grow abnormally.
| This report describes genetic variants associated with Extranodal natural killer T-cell lymphoma (NKTCL). This aggressive blood cancer grows outside of the lymphatic system, usually in the nose. |
Non-Hodgkin lymphoma starts in either B cells or T cells, which are immune cells that help make antibodies in the immune system. This type is more common than Hodgkin lymphoma. There are many subtypes of non-Hodgkin lymphoma, with diffuse large B-cell lymphoma and follicular lymphoma being the most common.
Hodgkin lymphoma is similar to non-Hodgkin lymphoma in that it affects the B cells of the lymphatic system. In this case, patients also experience large lymphocytes called Reed-Sternberg cells in their lymph nodes. Most people are diagnosed either in their 20s or after the age of 55. It is slightly more common in males than females.
Myeloma blood cancer
This condition occurs in the blood’s plasma cells, a special type of white blood cell that makes antibodies. This cancer of the plasma causes myeloma cells to crowd out healthy cells in the bone marrow. Because it is usually present in many parts of the bone marrow, it is called multiple myeloma. This type of blood cancer usually occurs in males over the age of 60. It is twice as prevalent in African Americans as those of other races. It is also more common in patients with monoclonal gammopathy of undetermined significance (MGUS) or solitary plasmacytoma.
Current Research on Blood Cancer [Updated August 2021]
There has been an increase in the study of blood cancer treatments in recent years, and this has led to improvement in the survival rate of patients suffering from the condition.
In 2016, a clinical trial co-led by a Dana-Farber researcher confirmed that a new oral targeted drug encourages anti-cancer activity in patients with resistant or relapsed acute myeloid leukemia (AML). According to Dr. Anthony Letai, senior author of the report, the drug, termed ABT-199, blocks the cancer cells’ mechanisms that allow them to survive.
In another clinical trial, the ABT-199 was said to improve outcomes in patients with a hard-to-treat form of chronic lymphocytic leukemia (CLL). At the time of the result, the researchers were enthusiastic that the drug was expected to gain FDA approval the following year. The brand name drug Venclexta was approved for both AML and CLL in April 2016.
Other research in December 2016 led to researchers concluding that new immunotherapy drugs, which had shown dramatic results in melanoma, were confirmed to also show promising results for people with blood cancers. Researchers reported that 87 percent of patients with resistant forms of Hodgkin lymphoma achieved complete or partial remission after taking the immunotherapy agent, Nivolumab. Many of these patients had previously had stem cell transplants and treatment with several drugs. A follow-up to the result showed that most of the patients who responded positively to the drug did not experience relapse a year after the treatment.
In 2020, a study named “Continued Long Term Responses to Ibrutinib + Venetoclax Treatment for Relapsed/Refractory CLL in the Blood Cancer UK TAP Clarity Trial” saw researchers study how the combination of two drugs helped to treat relapsed/refractory CLL. The research/trial was carried out on 50 patients and the results achieved were of the following:
Of the 50 evaluable patients recruited to the study, 23 patients stopped both treatments at or before Month 38. The majority cited improvement (17 of 23) before the 38th month. Meanwhile, 27 of 50 patients were still receiving at least one trial treatment at this time point, with the response data of 11 patients still pending. None of the treatments showed any considerable side effects, with most reactions classified as mid or manageable.
The researchers concluded that the drugs improved treatments in patients since patients’ response to the combination treatment was sustained. They also concluded that the initial rate of disease depletion is highly predictive of longer-term response to combination treatment in relapsed/refractory CLL. Patients who did not show rapid disease clearance and had persistent disease after 12 months of combination treatment were found to have stable or slowly decreasing disease levels akin to that seen when only taking one therapy.
Risk Factors for Blood Cancer
All cancers are caused by some gene mutation, but not all of them are hereditary. Genetic mutations can be caused by environmental or lifestyle factors with no family history. The American Cancer Society provides an outline of the known risk factors for blood cancers.
Radiation
Radiation exposure is a known risk factor for ALL and AML, the two types of acute leukemias, and non-Hodgkin lymphoma. For example, the survivors of the Japanese atomic bomb attacks have a much higher risk of developing these types of cancer.
Besides age and gender, radiation is the only other risk factor for CML.
Many cancers are treated with a combination of radiation and chemotherapy. Unfortunately, in some cases, this radiation exposure increases the chances of developing leukemia.
Other forms of radiation, such as x-rays and CT scans, are only thought to present a very small risk if any at all. Still, most doctors try to limit radiation exposure, especially in children and pregnant women.
Chemicals
Long-term exposure to chemotherapy drugs or other chemicals such as benzene may increase blood cancer risk, especially the acute leukemias ALL and AML and non-Hodgkin lymphoma. Benzene is an industrial solvent used to produce other products. It is also present in cigarette smoke and some household cleaners.

Some chemotherapy drugs seem to have an especially large effect on the development of AML. Drugs called alkylating agents or others known as topoisomerase II inhibitors are linked to an increased risk of AML.
Some studies link exposure to Agent Orange, an herbicide used during the Vietnam War, as well as other commonly used pesticides, to an increased risk of CLL. Research is still ongoing.
Viral infections
Although certain viral infections can cause some blood cancers, these tend to be rare in the United States. In Africa, the Epstein-Barr virus (EBV) has been linked to Burkitt lymphoma (a non-Hodgkin lymphoma), Hodgkin lymphoma, and to a form of ALL. Usually associated with “mono,” the virus has also been linked with a type of lymphoma that can occur after a stem cell transplant.
Human T-cell lymphotropic virus (HTLV-1) also increases the risk of ALL, mainly outside of the United States, and non-Hodgkin lymphoma.
Smoking
Tobacco smoke is linked with many cancers, especially in the lung and mouth. However, it is also a known risk factor for others, including blood cancers such as AML.

Certain blood disorders
Some patients with lingering blood disorders are at a greater risk for AML. These conditions include chronic myeloproliferative diseases such as polycythemia vera, essential thrombocythemia, and idiopathic myelofibrosis. Another disorder called myelodysplastic syndrome (MDS), which leads to low blood cell counts and abnormal cells in the bone marrow, is also a risk factor.
Weakened immune system or autoimmune diseases
Patients with a weakened immune system have shown a greater risk of developing both non-Hodgkin and Hodgkin lymphoma. Those who undergo organ transplants may be taking medications to prevent their immune system from rejecting the new organ. This immune depression can increase the risk. Other conditions, such as HIV or the inherited disorders ataxia-telangiectasia (AT) and Wiskott-Aldrich syndrome, weaken the immune system enough that increased risk of non-Hodgkin lymphoma is a concern.
Autoimmune disorders occur when the body’s immune system mistakenly attacks healthy cells in different parts of the body. Rheumatoid arthritis, systemic lupus erythematosus (SLE or lupus), Sjogren disease, and celiac disease are the most common disorders linked with an increased risk.
Obesity
Being obese or overweight contributes to a number of general health issues. It is also associated with an increase in the risk of multiple myeloma.
Genetic disorders
Some blood cancers are associated with family history. For example, AML, non-Hodgkin lymphoma, and myeloma are hereditary cancers known to run in families where you are more likely to develop the disease if a close family member also has it. Others, such as CLL and CML, appear to have no connection to inheritance. There are also some genetic disorders that seem to be linked with an increased risk of developing certain blood cancers.
ALL
- Down syndrome
- Klinefelter syndrome
- Fanconi anemia
- Bloom syndrome
- Ataxia-telangiectasia
- Neurofibromatosis
- Li-Fraumeni syndrome
AML
- Fanconi anemia
- Bloom syndrome
- Ataxia-telangiectasia
- Diamond-Blackfan anemia
- Shwachman-Diamond syndrome
- Li-Fraumeni syndrome
- Neurofibromatosis type 1
- Severe congenital neutropenia (also called Kostmann syndrome)
- Down syndrome (being born with an extra copy of chromosome 21)
- Trisomy 8 (being born with an extra copy of chromosome 8)
Genetic testing can help you assess whether you or your family is at risk for these conditions.
Some forms of blood cancer have proven to be treatable and clinical trials are ongoing to further improve the prognosis. You may be interested in checking out the leukemia & lymphoma society for further information on disease, support resources, and the most up to date research.
Looking for more information on cancer and genetics? Check out our other articles on pancreatic cancer and thyroid cancer, among others!
You can also see our posts in the Genetic Cancer Testing series and explore the Nebula Research Library to learn about hundreds of other conditions influenced by genetics, including many cancers.
