Table of contents
Nebula Genomics DNA Report for Tourette’s
Is Tourette’s genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

| This information has been updated to reflect recent scientific research as of July 2021. |
What is Tourette’s?
Tourette syndrome (TS), or Tourette’s, is a congenital disorder of the nervous system. Involuntary movements (called tics, from the French tic ‘nervous twitching’) and also tic-like outbursts of sound are the main characteristics. Doctors characterize Tourette syndrome and tic disorders as sudden, uncontrolled, repetitive, rapid, and unwanted movements or sounds. Symptoms typically appear in childhood and vary in severity throughout life.
Simple motor tics may manifest as eye blinking, nasal blinking, head tossing, or grimacing. In the motor domain, the category of complex tics includes imitative grimacing and imitating the actions of others.

Examples of simple vocal or phonic tics include emitting meaningless sounds, coughing, or imitating animal sounds. Complex vocal tics involve repeating words or blurting out obscene and aggressive expressions.
The first signs are usually simple motor tics in the head and neck region. The tics become more severe as children mature into their teens, but symptoms typically improve by the early 20s. In some cases, the tics disappear completely. The condition does not tend to get worse with age, and most individuals with Tourette’s can live normal lives.
There is no cure or treatment for the cause of primary tic disorders, although treatments for some of the symptoms are available.
The term names the French neurologist and psychiatrist Georges Gilles de la Tourette, who first described the clinical picture around 1884 at the suggestion of his teacher Jean-Martin Charcot. Sometimes experts refer to the disorder as Gilles de la Tourette syndrome.
Is Tourette’s Genetic?
Is Tourette syndrome genetic? Studies indicate that TS is inherited as a dominant gene. Notably, about a 50% chance of parents passing the gene on to their children. Other research suggests that the genetic contributions are more complex than a single hereditary gene. Evidence for this theory is children who develop the symptoms without a parent also having the condition.
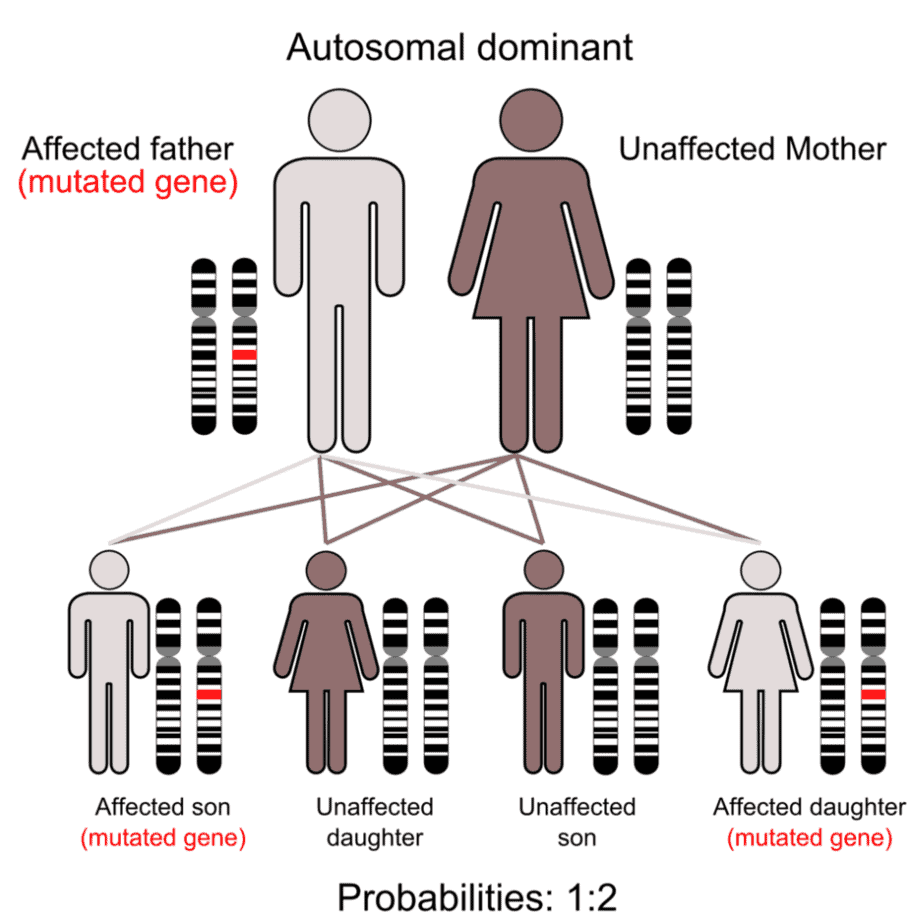
Experts have identified susceptibility genes involving the SLITRK1 gene in a small number of people with TS. While some cases of Tourette’s may involve this gene, direct causal links cannot be explained, and most experts believe that other genetic factors are involved in the majority of cases.
This gene provides instructions for making a protein that is active in the brain. The protein made with the instructions of this gene probably plays a role in the development of nerve cells, including the growth of axons and dendrites that allow each nerve cell to communicate with nearby cells.
The discovery of additional genetic mutations associated with the condition is an active area of research.
Current Research on Genetic Tourette’s [Updated July 2021]
Researchers carried out one of the earliest studies on this congenital disorder—Tourette’s—in 2019. In this research study, they used a genome wide association study to determine the genetic influence of Tourette’s syndrome. Hence, the unknown genetic orientation of Tourette’s syndrome began to come into the light.
Individuals diagnosed with Tourette’s syndrome provided the polygenic risk scores (PRSs) studied in this research. Ultimately, the result showed that people with certain genetic variants had a higher risk of developing the condition.
Researchers also found that Tourette’s is highly heritable. They discovered this through research designed to determine the genetic architecture of the condition, selecting almost 4000 individuals from the Tourette Syndrome Association International Consortium for Genetics for this study.
The study authors discovered two cross-disorder symptom-based phenotypes from the analysis of these discovery samples. They found that the level of heritability regarding Tourette’s syndrome to be extremely high and significant, showing that genetics plays a significant role in the Tourette’s experienced by individuals.
Since Tourette’s has heritable components, individuals who have parents with the disorder have a greater chance of having the condition themselves. This overview notes that the mutation of a single genetic factor may be associated with Tourette’s in some individuals. Therefore, children from a family with a mutation in the genes encoding the enzyme histidine decarboxylase (HDC), could be at a higher risk.
Epidemiology
The Centers for Disease Control and Prevention (CDC) conducted a study in 2016-2017 using parent-reported data. The results showed that 0.3% of children 6–17 years of age in the general population of the United States (135,000) had received a diagnosis of TS.
Out of all the cases reported from 2016-2017, 44% of them were moderate or severe. Doctors usually diagnose the condition in childhood. Notably, they diagnose adolescents between the ages of 12-17 twice as much as children ages 6-11. Boys were about three times more likely to have it than girls and there did not appear to be a difference between ethnic and socio-economic groups.
Symptoms
The presence of transient tics is the main symptom. Tourette’s syndrome is a complex disease that presents itself in a variety of ways. According to the NIH National Institute of Neurological Disorders and Stroke, the disorder is characterized by tics divided into either motor (movement) or vocal (sound) categories. These tics can be either simple or complex. Severity can range from very mild to severe, with most cases being mild.
Simple tics are sudden, brief, repetitive movements involving a limited number of muscle groups, while complex tics involve distinct, coordinated patterns of movement. Various symptoms of Tourette syndrome include:
Motor tics
Simple motor tics: eye blinking and other eye movements, facial grimacing, shoulder shrugging, and head or shoulder jerking.
Complex motor tics: facial grimacing combined with a head twist and a shoulder shrug. Patients may display other complex motor tics, which may appear to be done on purpose, include smelling or touching objects, bending, hopping, obscene gestures, or twisting.

Vocal tics
Simple vocal tics: throat clearing, coughing, barking, or grunting.
Complex vocal tics: repeating own words or phrases, repeating others’ words (echolalia) or phrases, or more rarely, using obscene, vulgar, or swear words (coprolalia).
Some patients describe an urge or sensation in the affected muscle group that can only be relieved by completing the tic.
Patients more easily trigger tics during times of high emotion, such as excitement or anxiety. Physical or auditory triggers can also trigger or worsen tics.
Although some patients are successful at suppressing or hiding their tics, this may result in a buildup of tension. Although tics may appear purposeful, they are always involuntary.
Among children diagnosed, 83% have also been diagnosed with at least one co-occurring condition. These disorders are usually additional mental, behavioral, or developmental disorder, including:
- Anxiety
- Attention Deficit Hyperactivity Disorder (ADHD)
- Oppositional defiant disorder (ODD) or conduct disorder (CD)
- Learning disabilities
- Developmental delays
- Autism spectrum
- Depression
- Speech or language problems
- Intellectual disabilities
- Obsessive compulsive disorder (OCD)
Causes of Genetic Tourette’s and Environment Factors
Although the exact cause of the condition is unknown, Tourette’s is most likely a combination of genetic and environmental factors. Because it is a neurological disorder, neurotransmitters such as dopamine and serotonin most likely play a role. Specifically, the condition is most likely involved with the breakdown of dopamine and abnormalities in certain parts of the brain such as the basal ganglia, frontal lobes, and cortex.
Risk factors include having a family history of the condition. Additionally, males are more likely to develop TS than females.
The CDC cites additional studies that associate certain environmental conditions before and after birth with the appearance of the disease. However, we need more research to confirm these initial findings. Some of these associations are:
- Smoking during pregnancy
- Pregnancy complications
- Low birth weight
- Infection
Diagnosis
There is no laboratory, blood, or imaging test that can diagnose Tourette’s. Instead, your doctor will rely on physical signs and symptoms.
According to Mayo Clinic, diagnosis is based on the following observable symptoms:
- Both the motor type of tic (at least two different kinds) and the vocal type of tics (at least one type) are present, although not necessarily at the same time
- Chronic tics lasting at least a year. Tics occur several times a day, nearly every day, or intermittently
- Tics begin before age 18
- Tics are not side effects of medications, other substances or triggered by another medical condition
- Tics must change over time in location, frequency, type, complexity, or severity
Your doctor will rule out other conditions that mimic observable tics before making a diagnosis of Tourette’s. These include vision problems as a cause of frequent eye blinking and allergies in the case of sniffling.
Treatment
There is no cure for Tourette syndrome. Treatment options are based on managing symptoms so that they do not interfere with daily life. These treatments are usually either medicine- or therapy-based.
Medications
Medications can help patients manage everyday life. However, it should be noted that most medications prescribed for Tourette’s have not been approved by the U.S. Food and Drug Administration (FDA) for treating tics.
This form of treatment is not effective for everyone. If the symptoms are mild enough, no treatment at all may be necessary.
Medications that block or lessen dopamine: Since the condition is most likely influenced by abnormal expression of neurotransmitters, reducing the impact of these chemicals often helps alleviate symptoms. Possible side effects include weight gain and involuntary repetitive movements. Certain types of these medications may also cause severe depression.
Botulinum (Botox) injections: An injection of this medication into the affected muscle might help relieve a simple or vocal tic.
ADHD medications: Stimulants used to treat ADHD can help patients with Tourette’s increase attention and concentration. However, for some patients, medications for ADHD can exacerbate tics.

Central adrenergic inhibitors: Doctors typically prescribe these medications for high blood pressure. They might help control behavioral symptoms such as impulse control problems and rage attacks. Side effects may include sleepiness.
Antidepressants: Doctors may prescribe these medications to treat the depression, anxiety, and OCD that may accompany the condition.
Antiseizure medications: Recent studies suggest that some people with Tourette syndrome respond to topiramate and levetiracetam, drugs used to treat epilepsy.
Therapy
This treatment is used to help control tics, specifically the frequency, severity, and impact of Tourette disorder on motor and vocal tics. Support groups are also a valuable resource for people with this condition.
Behavior therapy: Cognitive Behavioral Therapy (CBT) for tics, including habit-reversal training, can help monitor tics, identify premonitory urges, and learn to voluntarily move in a way that’s incompatible with the tic.
Habit reversal training is a type of behavioral therapy. It is divided into an awareness training portion and competing response training. The first part focuses on identifying the tic out loud when it is happening.
The second part involves creating a competing action when the urge to engage the tic occurs. For example, if the tic involves moving one’s hands to a certain area of the body, the competing action would involve moving the hands to a different area.
Psychotherapy: This approach is common when treating multiple conditions, including Tourette’s, ADHD, OCD, depression, or anxiety.
Deep brain stimulation (DBS): For severe tics that don’t respond to other treatments, DBS might help. A battery-operated medical device is implanted into the brain and delivers electrical stimulation to targeted areas that control movement. This is a new treatment still in the early research stages. More investigation is needed to determine if it is safe and effective.
Prognosis
Because symptoms largely subside in early adulthood, most people with Tourette’s go on to lead healthy lives.
Parent training can help families learn how to manage the symptoms and overcome social challenges. The CDC supports this type of training not just for Tourette’s, but for other disruptive behaviors, such as ADHD, as well. This training often covers positive reinforcement and discipline that is effective with a particular child. Parents can also take advantage of school resources to help their children succeed in social settings.
If you liked this article, you should check out our other posts in the Nebula Research Library!
September 23, 2022
