Table of contents
Nebula Genomics DNA Report for Vitiligo
Is vitiligo genetic? We created a DNA report based on a study that attempted to answer this question. Below you can see a SAMPLE DNA report. To get your personalized DNA report, purchase our Whole Genome Sequencing!

| This information has been updated to reflect recent scientific research as of May 2021. |
What is Vitiligo?
Vitiligo, also called white spot disease or checkered skin, is a chronic, non-contagious skin disease that affects about 0.5 to 2% of people worldwide. It causes white, pigment-free skin patches of vitiligo to appear on the skin, which can slowly expand but do not necessarily have to.
These patches can appear on any part of the body, and many people with the condition have them in multiple areas. Usually, they appear on both sides of the body. The affected regions first usually are those most exposed to the sun.
Types
The condition is classified as either segmental (unilateral) or non-segmental (bilateral), with the latter being the more common type.
Non-segmental vitiligo (also known as generalized vitiligo) means that the condition affects both sides of the body, such as hands or cheeks. The patches normally expand over time, and loss of pigment progresses in an on and off pattern.
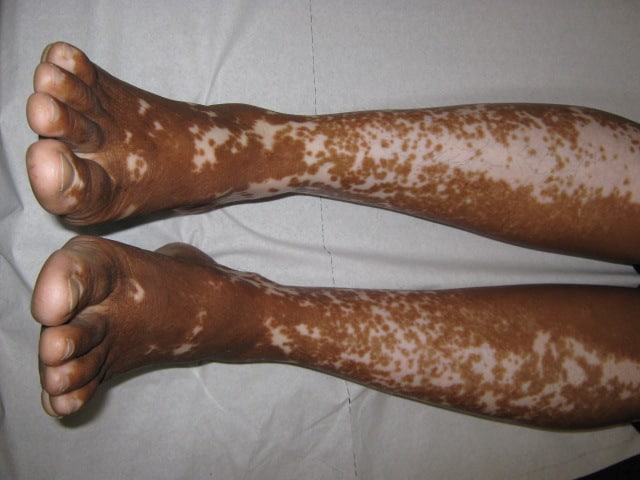
The segmental form only affects one side of the body, and the patches typically remain static after expanding for an amount of time. This type is diagnosed at an early age, and patients are more likely than the non-segmental group to also have changes in color to the hair. Only about 10% of all vitiligo cases are thought to be segmental.
A third type is known as focal vitiligo, which is when there are only a few spots located in a specific area of the skin.
More presentations of vitiligo can be found in a 2017 article published in the Journal of Academic Dermatology (DOI: 10.1016/j.jaad.2016.10.048).
Is Vitiligo Genetic?
The exact genetic cause is complicated as over 30 genetic components are thought to contribute to the increased risk of developing vitiligo. The two most important genes are NLRP1 and PTPN22.
Is vitiligo hereditary? It is known that vitiligo is hereditary or runs in families. About one-fifth of people with this condition have at least one close relative who is also affected.
The role of environmental triggers is highlighted when one considers that identical twins only have a 23% chance of both developing the condition.
NLRP1: The NLRP1 gene provides instructions for a protein involved in the immune system that helps regulate inflammation. Inflammation is a result of the immune system reacting to foreign invaders by sending signaling molecules and white blood cells to a site of injury or disease and facilitating tissue repair. After the issue has been controlled, the body normally stops the inflammatory response to prevent damage to its own cells and tissues.
PTPN22: The PTPN22 gene provides instructions for a protein involved in signaling that helps control the activity of immune system cells called T cells. T cells identify foreign substances and defend the body against infection.
Together, variations in the NLRP1 and PTPN22 genes affect the activity of the immune system, making it more difficult for the body to control inflammation and prevent the immune system from attacking its own tissues.
Other genes associated with the condition include those that control melanocyte formation and other autoimmune diseases.
Current Research on Vitiligo
Contrary to what many might believe, vitiligo is not a rare disease. In fact, it is one of the most common autoimmune diseases. So, it is no surprise that it has generated thousands of studies and articles.
In 2017, several medical schools from Taiwan made an assessment of vitiligo’s activity to determine its stability using Wood’s lamp. This research was performed as a follow-up to crafting procedure. Check out this article on Woods light (a form of ultraviolet light) to better understand what this procedure is about.
Another procedure to treat vitiligo, phototherapy, was highlighted in this study from 2017. The meta-analysis included 35 studies with 1428 patients.
As we mentioned earlier, conditions such as anxiety and depression prevail among vitiligo patients. This 2020 study digs deeper into the relationship between stress and vitiligo. This other research studies the connection between vitiligo and anxiety. Both studies seek to bring awareness of the need for proper management of patients with skin conditions.
There have also been studies about vitiligo causes. A meta-analysis of selenium levels in patients with vitiligo seeks to evaluate a relationship between those two. It is important to note that selenium deficiency has been known as a cause of autoimmune disease.
If you are interested in autoimmunity in segmental vitiligo, this 2020 article from Belgium and Croatian universities focuses on this topic. The autoimmune segmental vitiligo has only been recently understood, and this piece explains how it compares to non-segmental vitiligo, among other findings.
Funding for vitiligo research is very little, making it even more challenging to understand the disease better and find new treatments.
Epidemiology
People of any skin color can have the condition, but it is most noticeable in people with dark skin. Overall, it has a worldwide prevalence of 0.5-2%. That is roughly 70 million people on which vitiligo occurs.
The condition affects males and females equally and can affect any person at any age. The age of onset is usually before the age of 20. 20-35% of patients are children.
Symptoms
The most characteristic symptom of vitiligo is the appearance of lightened or white patches on the skin. The term for loss of skin color is called depigmentation. This is often the only symptom, although some patients describe the patches as itchy or painful.
While the patches most cause the skin to turn white, pigment can be lost at any part of the body, including skin, hair, eyes, mouth, and around body openings such as the genitals. Other patients experience premature lightening of hair on the scalp, eyelashes, eyebrows, or beard. The mucous membranes in the mouth and nose may also be affected.
While the physical signs of vitiligo may be minor and not life-threatening, a high percentage of people with it experience psychological distress such as depression due to patients being stigmatized. This effect on mental health can have a considerable impact on general well-being.
In addition to the segmental and nonsegmental types, the condition is further classified into subtypes that describe how much of the body is affected by depigmentation. These subtypes are localized (a few small patches limited to a few areas of the body), generalized (scattered patches), and universal (patches cover most of the body). Generalized is the most common form, while universal is the rarest.
A person with vitiligo is at an increased risk of sunburn, eye problems, and hearing loss, as well as pernicious anemia.
Causes
The exact vitiligo causes are unknown. Questions people usually ask include, “Are you born with vitiligo?” and “Can you develop vitiligo?” Vitiligo development is thought to be the result of genetic susceptibility triggered by environmental factors such as an autoimmune disease (e.g. Addison’s disease).
As a result, the condition destroys skin pigments, leading to pigment-free white patches.
Biologically, the white patches occur when pigment cells called melanocytes die prematurely or stop producing melanin. Some experts believe permanent or transient autoimmune blockage or destruction of melanocytes is part of the cause. The condition often co-occurs with other autoimmune disorders, which may be risk factors.
Stress could act as a trigger to vitiligo onset as its effects can disrupt the immune system. Other trigger events may be related to severe skin trauma or sunburn.
Risk factors
Those with a family history or certain autoimmune disorders tend to be at a higher risk of vitiligo. Some diseases such as rheumatoid arthritis, Hashimoto’s disease (a thyroid disease), alopecia areata (causes hair loss), and type 1 diabetes also appear to play a role in triggering the condition.
Diagnosis
A positive diagnosis can usually be made by physical examination alone. In most cases, your doctor will recommend seeing a dermatologist. Sometimes, if the specialist wants more information on how the condition affects your skin, they may recommend either a skin biopsy or a blood test.
Medical history is often the first step towards diagnosis. For instance, if you have a pre-existing autoimmune disease or if family members also have the condition, the appearance of white patches is most likely an indication of a positive diagnosis. The dermatologist will also physically examine your skin to determine the spotting pattern, which provides the subtype of the disease.
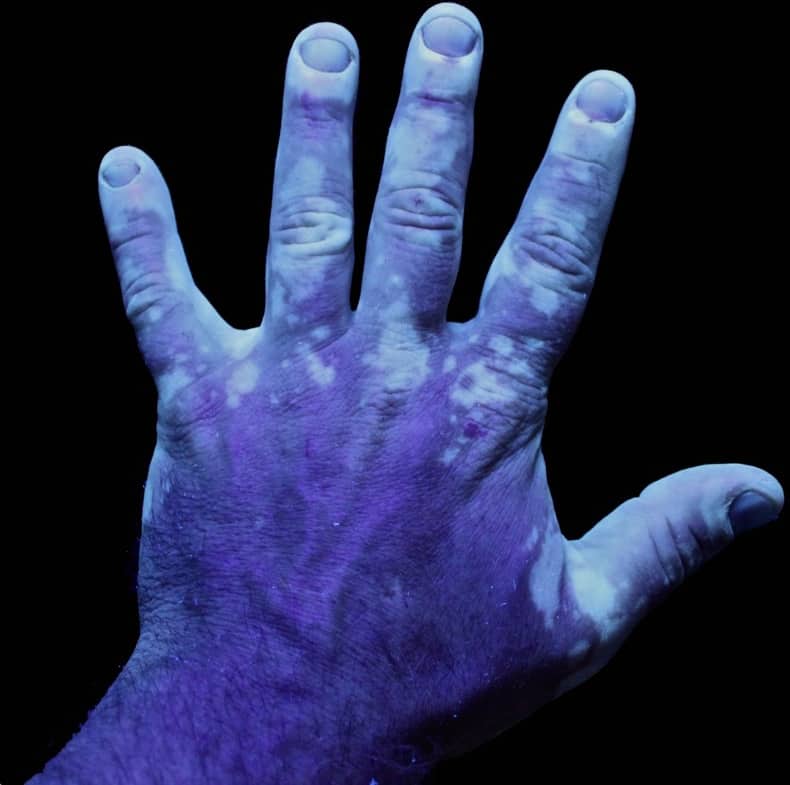
If you have lighter skin, the doctor may need an instrument such as UV light (black light) to determine the full extent of the pigmentation. UV light interacts with pigmented skin differently than depigmented skin.
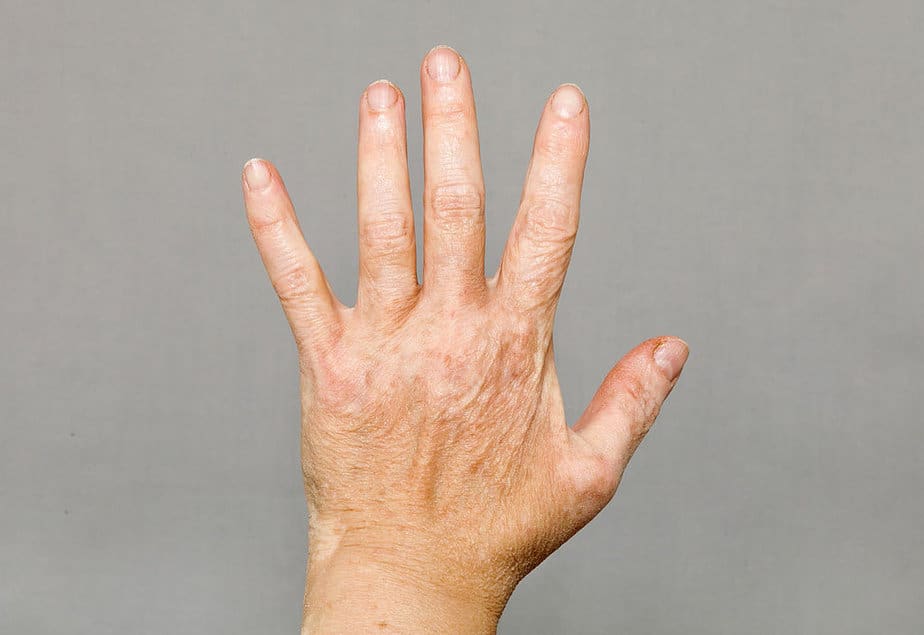
A skin biopsy can be performed to obtain additional information. This test can distinguish between melanocytes that are missing (a hallmark of vitiligo) and melanocytes that are damaged for some other reason. Very rarely, a skin cancer called hypopigmented cutaneous T-cell lymphoma (a type of blood cancer) can account for the white patches.
Blood tests are performed not to diagnose vitiligo but to obtain information regarding potential autoimmune complications or disorders that appear comorbid to the primary condition. A blood test for a thyroid condition is one of the more common tests.
Did you know that thyroid tests can be done at home? Learn more about at home thyroid tests!
Treatment
There is no cure for vitiligo, and some patients choose not to prevent vitiligo at all since it does not have any physical effects beyond changes in skin color. Support groups may help treat mental or psychological problems. Recommended treatment for vitiligo depends on age, how the condition progresses, and how much it affects your life, including your mental well-being.
The American Academy of Dermatology Association covers most of the treatment options available through health care professionals.
Patients who choose not to seek medical vitiligo treatment often use over-the-counter cosmetic products to cover the effects for a long term. These products include makeup, self-tanners, and skin dyes. This is often the safest method of treatment to improve quality of life and is usually advised for children.
Topicals
Several topical skincare treatments can be applied to help restore the color of vitiligo skin. The most commonly prescribed medicine is a corticosteroid of topical application. This treatment is most effective when the condition is in its early stages.
About half of patients regain at least some skin color after 4 to 6 months. These medicines have possible side effects, such as skin atrophy, when the skin becomes paper-thin, very dry, and fragile.
Another topical includes calcineurin inhibitors (TCIs) which inhibit T cell functions by blocking calcineurin. This treatment has been shown effective in treating the condition, especially when combined with light therapy.
Light therapy
This treatment uses ultraviolet B (UVB) light to restore the color in vitiligo skin. It may be more effective if combined with corticosteroids. Patients usually need to receive the treatment 2-3 times per week, and it may take months for the effects to be seen.
However, there are portable devices that patients can use at home. Side effects of this treatment include redness, itching, and burning. These side effects usually clear up within a few hours after treatment. Experimental treatment with UVA light may also be available.
Other options
Surgery: Surgery may be a last resort option for those who do not respond well to other options. Surgeries are designed to even out the skin tone by restoring color in affected areas.
Skin grafting is one option performed by replacing areas of lost pigment with segments of healthy, pigmented skin. Blister grafting is another option in which your doctor creates blisters on pigmented skin, usually with suction, and then transplants the tops of the blisters to discolored skin.
The final option is called cellular suspension transplant. In this procedure, the doctor takes some tissue from your pigmented skin, puts the cells into a solution, and transplants them onto the prepared affected area. Each of these surgeries comes with risks of scarring, infection, and failure of the skin to re-color.
You can learn more about vitiligo at the National Institute of Arthritis and Musculoskeletal and Skin Diseases website.
If you liked this article, you should check out our other posts in the Nebula Research Library, including other skin conditions such as psoriasis.
July 27, 2022
